Exposed Tooth Nerves: Causes, Instant Relief, & Treatment Options
 According to some studies, tooth sensitivity can affect up to 85% of adults.
According to some studies, tooth sensitivity can affect up to 85% of adults.
Healthy teeth shouldn’t cause pain. This is because the nerves inside the teeth are well-protected by strong layers of enamel and dentin.
When teeth become sensitive or painful—especially to cold, hot, or sweet foods and drinks—it’s a sign that something is wrong. This usually means the nerves are no longer fully protected and are exposed to the outside environment.
The result? Discomfort that can interfere with daily activities like eating, brushing, and even sleeping.
If this sounds familiar, don't worry. We'll explain the causes of exposed tooth nerves, tips for instant pain relief, and discuss the treatment options to help you manage this dental issue effectively.
In this article:
1. What Does It Mean When a Tooth Nerve Is Exposed?
2. Dental Conditions that Can Lead to Exposed Tooth Nerve
3. How Can Your Dentist Help Provide Relief?
4. Tips to Strengthen Teeth and Prevent Further Dental Issues
What Does It Mean When a Tooth Nerve Is Exposed?
Teeth are protected by two hard layers: the outer enamel and the underlying dentin.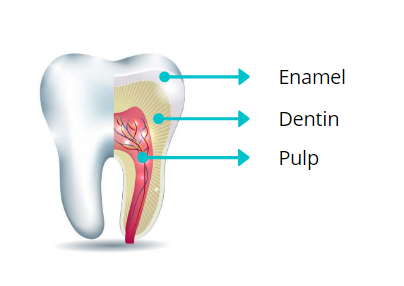
Enamel, the outermost layer, has no nerves. Its primary job is to perfectly shield the pulp—the inner part of the tooth that contains nerves and blood vessels—helping to prevent sensitivity, infections, and other dental problems.
Beneath the enamel is the dentin layer which also lacks nerves. However, it contains thousands of microscopic pores or channels called dentinal tubules, which connect directly to the nerves (as shown below).
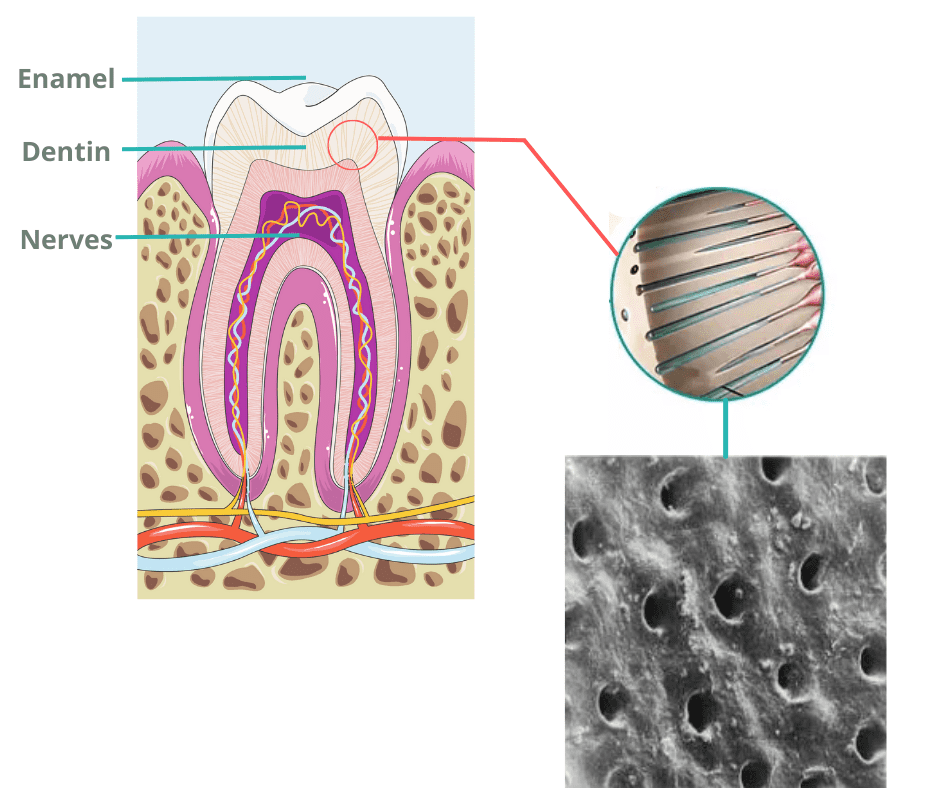
When enamel wears down and dentin becomes exposed, stimuli from food and drinks can travel through these tiny tubules and reach the nerves, triggering the sharp, short pain many people recognize as tooth sensitivity.
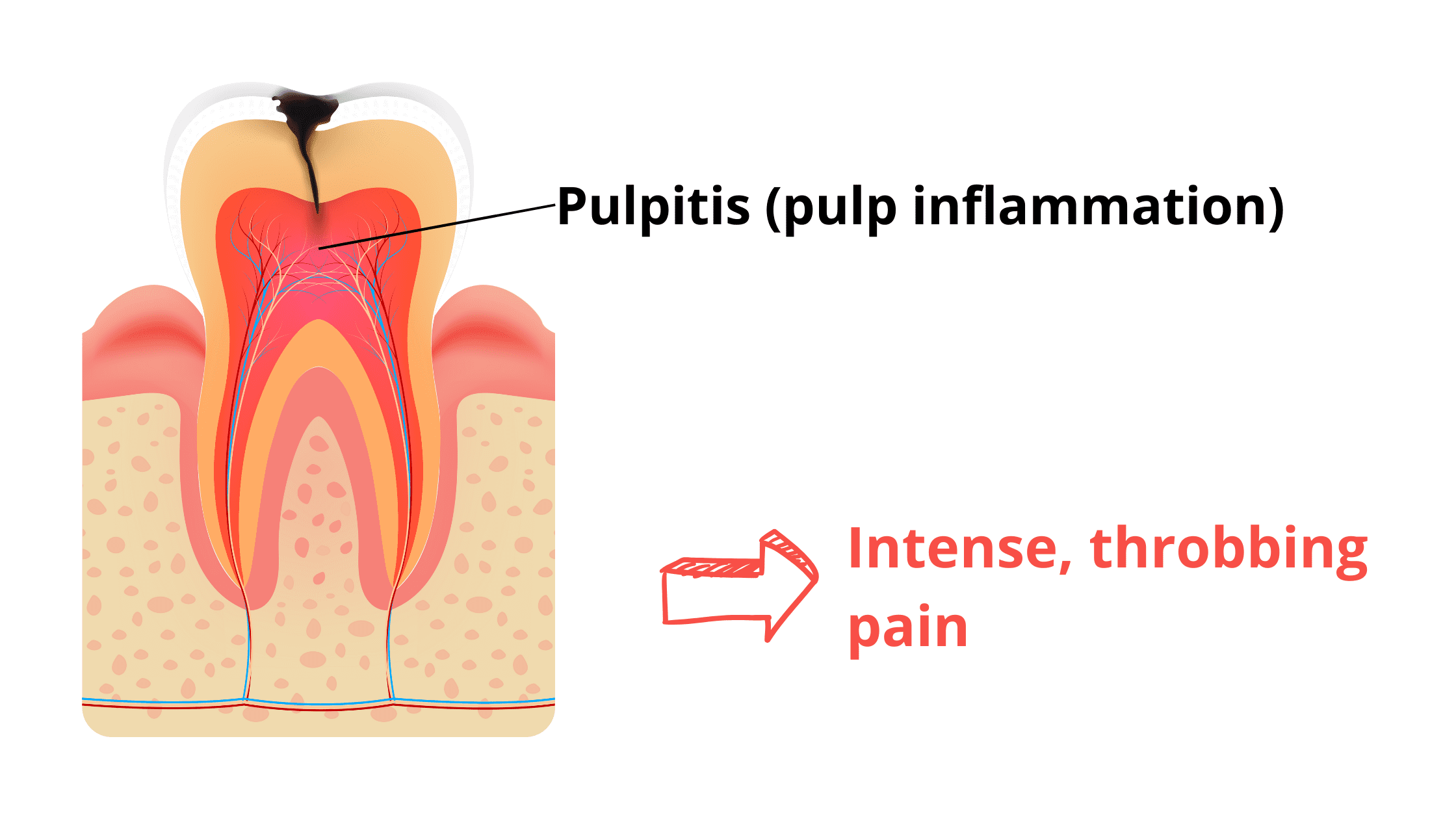
If the dentin itself starts breaking down, the nerves can become directly exposed to the bacteria-rich environment of the mouth. This is a much more serious condition that can cause severe inflammation and intense, throbbing pain.
Dental Conditions that Can Lead to Exposed Tooth Nerve
Exposed tooth nerves can be the result of many dental conditions. The most common include:1. Receding Gums
Receding gums occur when gum tissue gradually pulls away from the teeth, exposing the roots and sometimes making your teeth appear longer than before.

When the roots of your teeth become exposed, they often feel more sensitive to pressure from chewing, as well as to hot, cold, or acidic foods and drinks.
Why? Because roots don’t have enamel—they’re made entirely of dentin. And, unlike enamel, dentin isn’t built to handle the harsh environment of the mouth. That’s why once gums recede, sensitivity often follows.
The bigger problem is that exposed roots are far more vulnerable. They can wear down and decay much faster than the enamel-covered parts of your teeth.
Even worse, roots have a rougher surface that traps plaque more easily and makes them harder to keep clean.
That's why people with receding gums need to be extra careful and consistent with their oral hygiene.
Tips to Relieve Sensitivity and Pain from Receding Gums
The first step is to see your dentist to figure out why your gums are receding. The two major causes are plaque-related gum disease and trauma. You first need to fix these underlying issues to prevent further damage.
In the meantime, here are some tips to help soothe sensitive roots:
- Use a softer toothbrush: Switch to a toothbrush with soft bristles to avoid further irritation.
- Brush gently with proper technique: Avoid aggressive brushing, which can worsen gum recession. Use small, gentle circular motions and brush along the gum line to both clean the area and stimulate healthy blood flow.
- Avoid harsh foods and drinks: Limit hot, cold, acidic, or sweet items, as they can trigger or worsen sensitivity.
- Use desensitizing products: Apply a desensitizing toothpaste or a numbing gel directly to the exposed roots and let it sit for a few minutes so the active ingredients can take effect. Spit out the excess, but avoid eating or rinsing for at least 30 minutes.
Some options include:- Orajel (numbing dental gel)
- Hello Sensitivity Relief Toothpaste
- Sensodyne Pronamel Toothpaste
- Colgate Sensitive Prevent & Repair Toothpaste
2. Tooth Wear
Tooth wear is a common condition that gradually breaks down the protective outer layers of your teeth, making them thinner over time.
It usually progresses so slowly that you might not even notice it until half of your teeth are already worn down.
The two main factors behind tooth wear are:
- Mechanical Factors: Abrasive actions, such as brushing too hard or grinding your teeth (bruxism), can gradually wear down enamel. Over time, this can lead to tooth sensitivity and other dental problems.
- Chemical Factors: Acidic substances can erode enamel, making it thinner and more vulnerable. This may result from abusing acidic foods and drinks or medical conditions like gastroesophageal reflux disease (GERD), which exposes teeth to stomach acid.
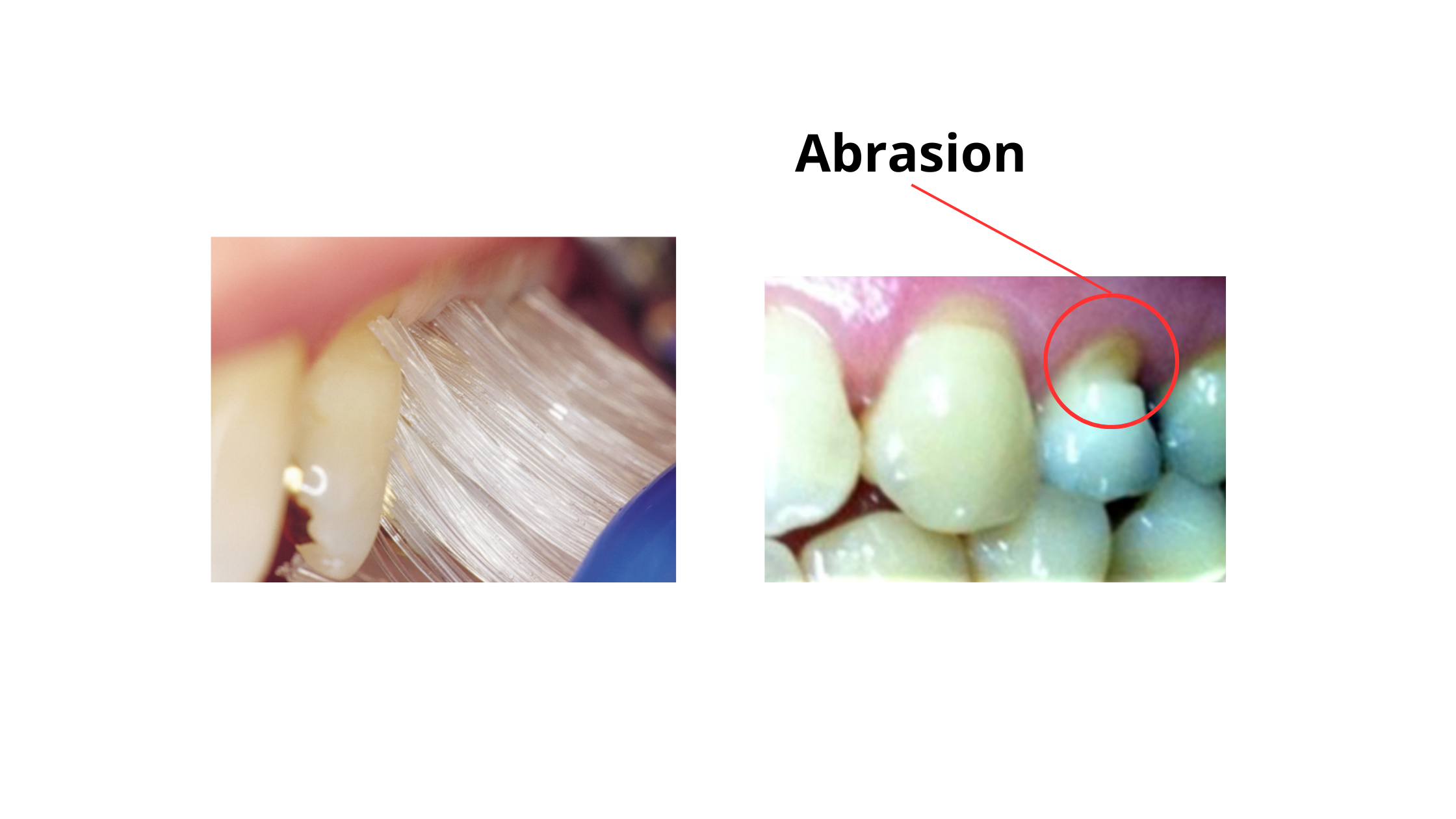
Tooth wear caused by brushing too hard
Relieving Pain from Tooth Wear
- Address the Root Cause: The first step is to eliminate the factors contributing to tooth wear. This can include:
- Brush gently using a soft toothbrush.
- Limit your intake of acidic and sugary foods and drinks.
- If you have dry mouth, stay hydrated and chew sugar-free gum between meals to stimulate saliva production.
- Get a custom nightguard if you grind your teeth to prevent further damage.
- Symptomatic Treatment (For Pain Relief): Use desensitizing gels and toothpastes (like the ones mentioned above) to help reduce sensitivity and provide relief.
- Remineralizing Treatment: This involves supplying your teeth with minerals to strengthen enamel and seal off exposed dentin, which can further reduce sensitivity.
Some great remineralizing products to complement your oral hygiene include Mi-Paste, GC Tooth Mousse, and CariFree Gel. - Professional Treatment: Once the condition is stable and the underlying causes are under control, your dentist can restore worn teeth using options like composite bonding, veneers, or crowns.
3. Tooth Decay
Tooth decay occurs when bacteria in the mouth break down sugars from the foods we eat and produce acids. These acids gradually erode enamel and dentin, eventually leading to cavities—deep holes in the tooth.
If left untreated, the decay can reach the nerves inside the tooth, causing severe inflammation and intense, stabbing pain that can even keep you awake at night.
However, tooth decay doesn’t need to get that deep to cause problems. Once it reaches the dentin, you may start experiencing sensitivity, particularly to hot or cold foods.
What to Do Right Away If You Have a Cavity
Cavities should never be ignored. Not only can they not heal on their own, but they can also worsen and lead to serious complications if left untreated.
Here’s what you should do:
- Schedule an appointment: You cannot treat a cavity on your own. The only way to fix it is for your dentist to remove the decayed tissue and restore your tooth properly.
- Take OTC pain relievers: Over-the-counter painkillers can provide temporary relief in the meantime.
- Rinse with warm saltwater: Mix 1 teaspoon of salt in a glass of warm water and rinse several times. This helps keep your mouth clean and soothes inflammation.
- Swish with clove oil: Dilute clove essential oil with a carrier oil and apply it to the painful area. Clove oil has natural numbing properties.
- Brush gently: Avoid harsh brushing to prevent increasing the pain.
- Avoid foods that can worsen the pain: Stay away from very cold, hot, spicy, or acidic foods and drinks.
4. Tooth Crack or Fracture
A cracked or fractured tooth can happen to anyone—whether from trauma, injury, or because the tooth is weakened by a cavity.
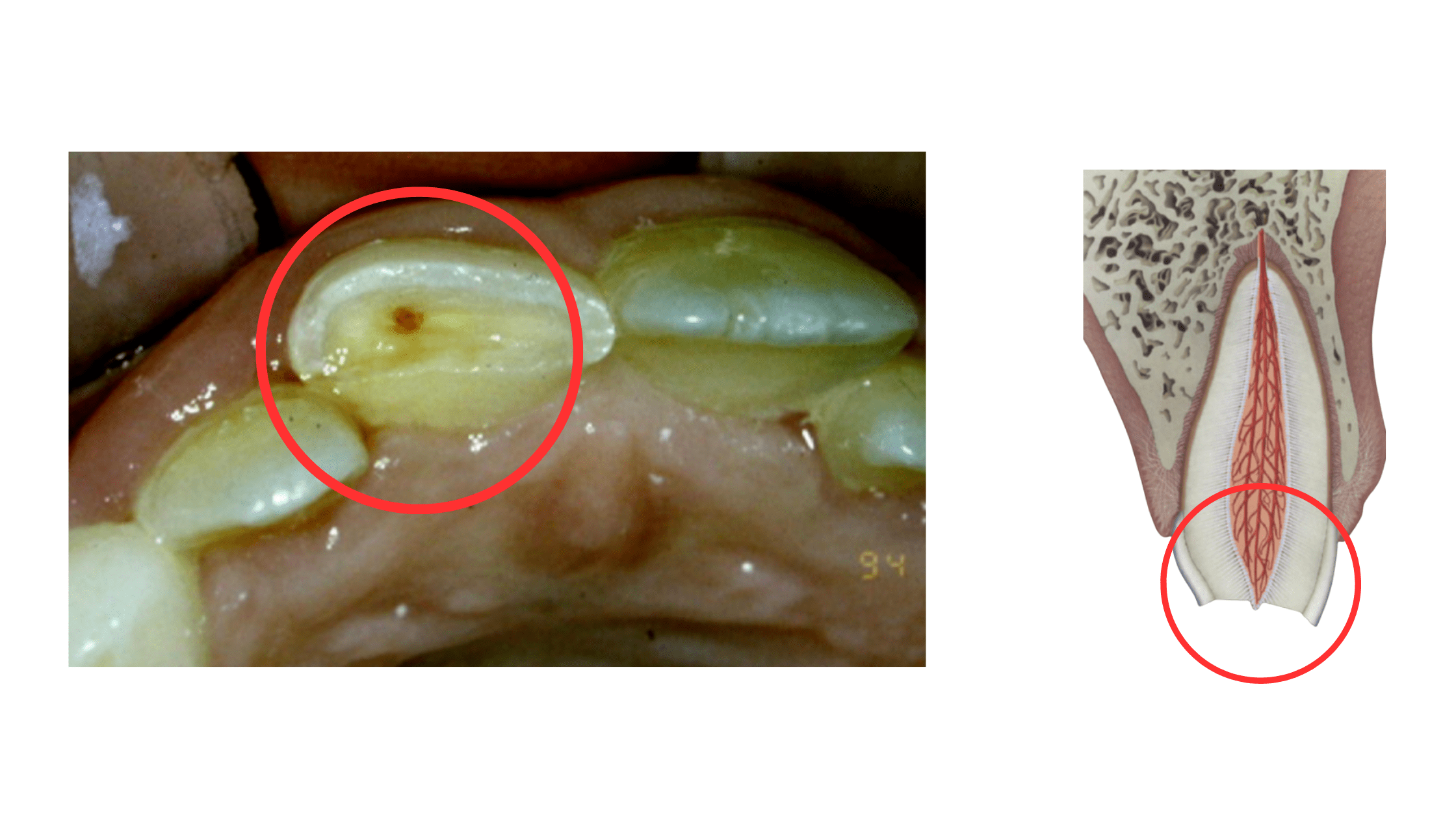
It’s crucial not to delay treatment, as the fracture or crack can create an entry point for bacteria and saliva to reach the nerves, potentially leading to a severe tooth infection.
These injuries can be tricky at first and hard to spot. Signs to watch for include:
- Dark lines on the tooth
- A loose fragment
- Sharp edges that weren’t there before
- Pain when biting down and releasing
- Swollen gums near the tooth
Relieving Pain from Fractured Teeth
If you suspect you have a cracked or fractured tooth, don’t wait it out. Seek treatment as soon as possible—the longer you wait, the more complex the treatment becomes, and the higher the risk of losing the tooth.
In the meantime, here's what you can do to manage discomfort:
- Avoid chewing on the painful side
- Stick to a soft, easy-to-chew diet
- Take OTC painkillers as needed
- Rinse with warm salt water or swish diluted clove oil
- Avoid anything that can worsen the pain
How Can Your Dentist Help Provide Relief?
If the pain is intense or persists despite your best efforts, it’s important to see your dentist, as it could be a more serious issue that requires professional care.Once the underlying cause is addressed, your dentist can use advanced techniques to numb the exposed nerves and provide lasting relief. Options include:
- Numbing Agent: Your dentist may apply a strong numbing agent to block the nerve pathway.
- Fluoride Varnish: It's a highly concentrated fluoride product (about 20 times more than toothpaste) that helps seal exposed dentinal tubules, thus reducing sensitivity.
- Dental Bonding: Dental bonding involves using a tooth-colored resin to cover and protect the exposed area.
- Laser Therapy: Laser treatment is another approach that helps seal exposed dentinal tubules, reducing sensitivity and pain.
- Gum Grafting: Your dentist may suggest a gum graft to cover the exposed roots.
- Root Canal Treatment: If the pain is severe, doesn’t respond to treatment, or the tooth nerve is badly damaged, a root canal may be necessary to remove the damaged nerve and provide long-lasting relief.
Tips to Strengthen Teeth and Prevent Further Sensitivity
1. Oral Hygiene:
- Brush your teeth at least twice a day with fluoride toothpaste, using a soft-bristled toothbrush and gentle, circular motions.
- Floss daily to clean between teeth and remove plaque from areas that your toothbrush cannot reach.
- Visit your dentist regularly for professional cleanings and check-ups to detect and address any dental issues early on.
2. Diet:
- Limit sugary and acidic foods and beverages that fuel the bad bacteria behind cavities.
- Make sure your diet provides all the essential vitamins and minerals needed for strong teeth and healthy gums.
- Drink plenty of water throughout the day to offset acidity and prevent dry mouth.
3. Promote Your Saliva:
Saliva is your mouth’s natural cleaner—it helps fight bacteria and wash away food debris.
On top of that, it’s packed with minerals that your teeth need to remineralize and repair themselves. Here are some tips to promote healthy saliva production:
- Chew sugar-free gum between meals: This helps stimulate saliva flow, which neutralizes acids and protects your teeth from decay.
- Avoid snacking between meals: Saliva does most of its job between meals, so give it a chance to protect your teeth by limiting frequent snacking.
- Stay hydrated and eat a balanced diet: Good saliva production, packed with essential minerals, starts with proper hydration and a nutrient-rich diet.
4. Consider Remineralizing Treatments:
These are add-ons to your oral hygiene routine and should never replace regular brushing and flossing.
When used consistently, they can effectively strengthen your enamel and prevent dental issues like cavities and sensitivity.
Remineralizing products can be either fluoride-based or fluoride-free:
- Fluoride-free options: CariFree Fluoride Free Gel (hydroxyapatite-based) | ROCS Tooth Gel
- Fluoride-based options: Mi-Paste Cream | ACT Anticavity Fluoride Rinse
Sources:
- Dentin Hypersensitivity: Etiology, Diagnosis and Treatment; A Literature Review - PMC (nih.gov)
- The etiology and prevalence of gingival recession - ScienceDirect
- Etiology and occurrence of gingival recession - An epidemiological study - PMC (nih.gov)