My Actual Risk of Nerve Damage After Wisdom Teeth Removal
The procedure of wisdom teeth removal can be challenging, but for most people, the recovery is smooth, and complications are uncommon.
One of the rare complications, however, is nerve injury. This can cause unusual sensations in your jaw, lips, or tongue. Most of the time, the effects are mild and temporary, but if the nerve is severely damaged or severed altogether, the symptoms may be long-lasting or even permanent.
In this article, we’ll break down the risk of nerve damage during wisdom tooth removal, the symptoms you should watch for, and the treatment options available.
One of the rare complications, however, is nerve injury. This can cause unusual sensations in your jaw, lips, or tongue. Most of the time, the effects are mild and temporary, but if the nerve is severely damaged or severed altogether, the symptoms may be long-lasting or even permanent.
In this article, we’ll break down the risk of nerve damage during wisdom tooth removal, the symptoms you should watch for, and the treatment options available.
In this article:
1. What’s Your Risk of Nerve Damage During Wisdom Tooth Removal?
2. How is the Risk Properly Assessed?
3. What Nerves are More Likely to be Affected?
4. What type of nerve damage can occur in wisdom tooth extraction?
5. I feel a tingling sensation after anesthesia. Is this normal?
6. What are the most common symptoms?
7. Can nerve damage lead to facial paralysis?
8. When does recovery from nerve damage usually occur?
9. Nerve damage treatment
10. Should wisdom teeth that carry a risk be left in place?
What’s Your Risk of Nerve Damage During Wisdom Tooth Removal?
What exactly is nerve injury or damage?During a wisdom tooth removal, there is a rare but potential risk where a crucial nerve may be damaged or, in extreme cases, cut completely. This can cause odd sensations, often felt as numbness, tingling, or a prickling feeling in parts of the face and mouth.
The symptoms you may notice can point to different conditions, including:
- Paresthesia — changes in sensitivity, like tingling or prickling
- Dysesthesia — burning sensations or pain
- Anesthesia — complete loss of sensation
Now, back to our question: How likely is nerve damage during wisdom tooth removal?
Your risk depends on several factors, including whether it’s an upper or lower wisdom tooth, if it’s impacted, how close it is to a nerve, and even your age.
-
Tooth position and nerve proximity:
This is the biggest factor. If the nerve lies far from your tooth, the risk is almost zero. But if the tooth sits too close, removing it without at least touching the nerve can be challenging. In the image below, you can see how close the nerve can be, even overlapping with the tooth roots.
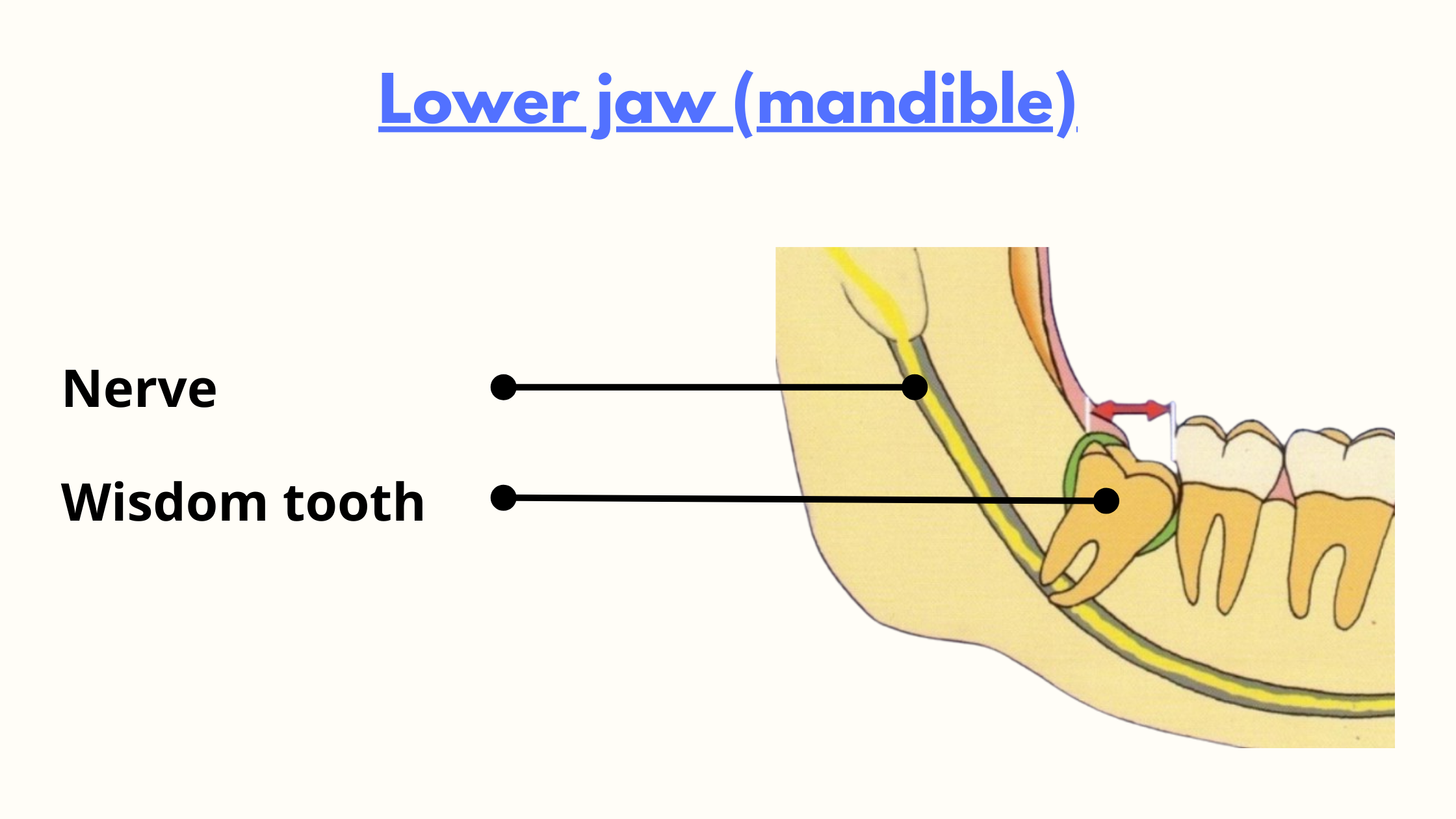
-
Impacted vs. fully erupted wisdom tooth:
The deeper the tooth is embedded in the jawbone, the harder the extraction and the higher the chance of nerve injury. -
Upper vs. lower wisdom teeth:
Lower wisdom teeth are trickier because they’re located near the major nerves of the jaw. -
Age:
The best time to remove wisdom teeth with the lowest risk of complications is usually before age 25. At that stage, the roots are still forming, and the bone is softer, making the procedure straightforward. After 25, the roots are fully grown, and the jawbone becomes denser, which makes extraction more complex and riskier.
What do the studies say?
According to many studies, the overall risk is relatively low, ranging between 0.35% to 8.4% (1,2).
Even if a nerve is damaged, most cases are temporary and typically resolve themselves after a few weeks or months.
Permanent sensory disturbances are exceptionally rare, accounting for no more than 2% of all cases (1).
How is the Risk Properly Assessed?
To assess the risk of nerve damage, we often rely on two main imaging tools: Panoramic X-rays and CBCT scans.On a panoramic X-ray, if the nerve runs very close to the tooth, it may show up as a deviated or uneven line, or as a dark shadow across the root tips (as shown below). This suggests that the nerve and tooth roots overlap.
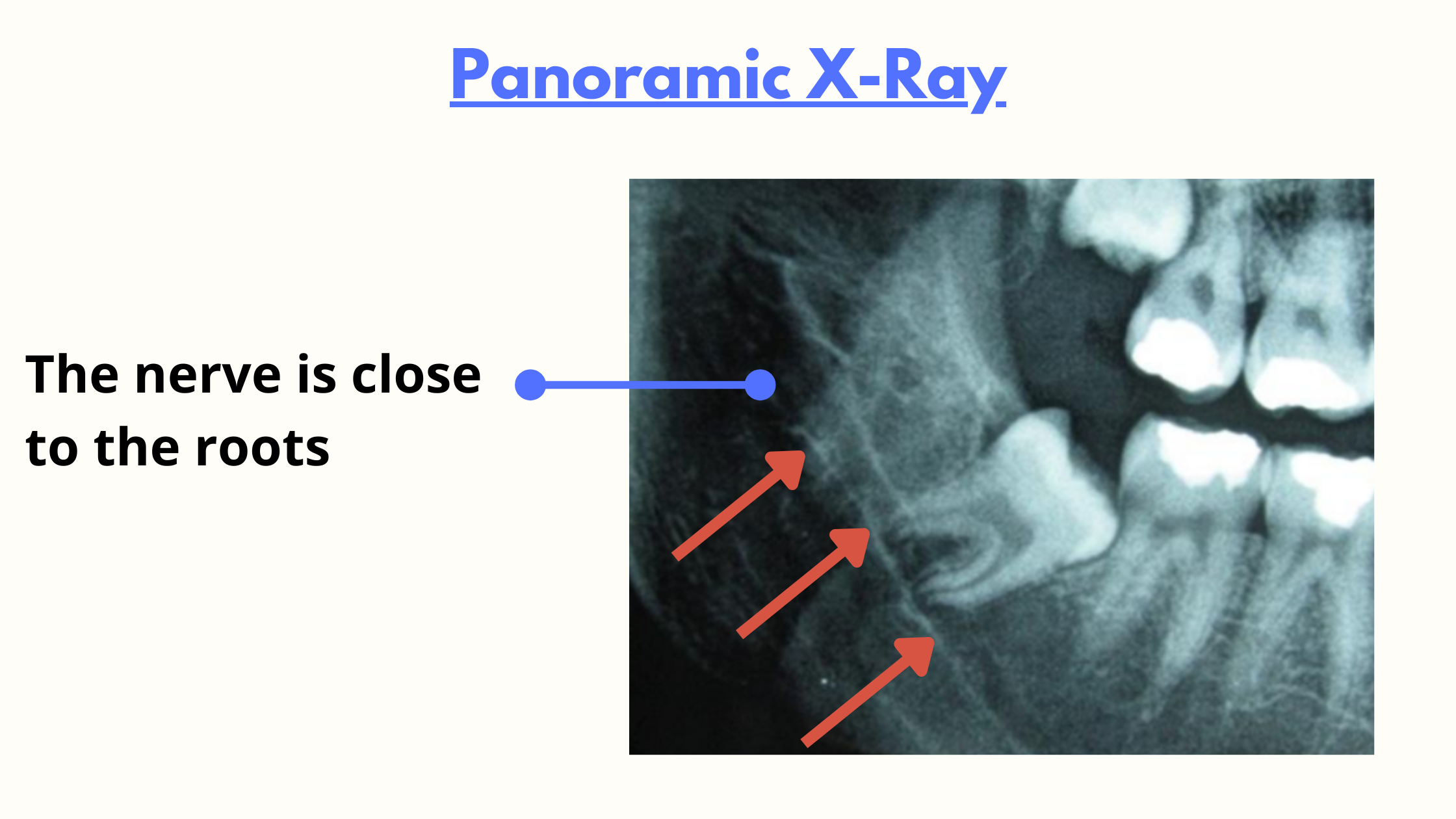
When the panoramic X-ray doesn’t provide enough detail, we turn to the CBCT scan. This 3D imaging offers a more accurate three-dimensional view of the tooth, bone, and nerve position.
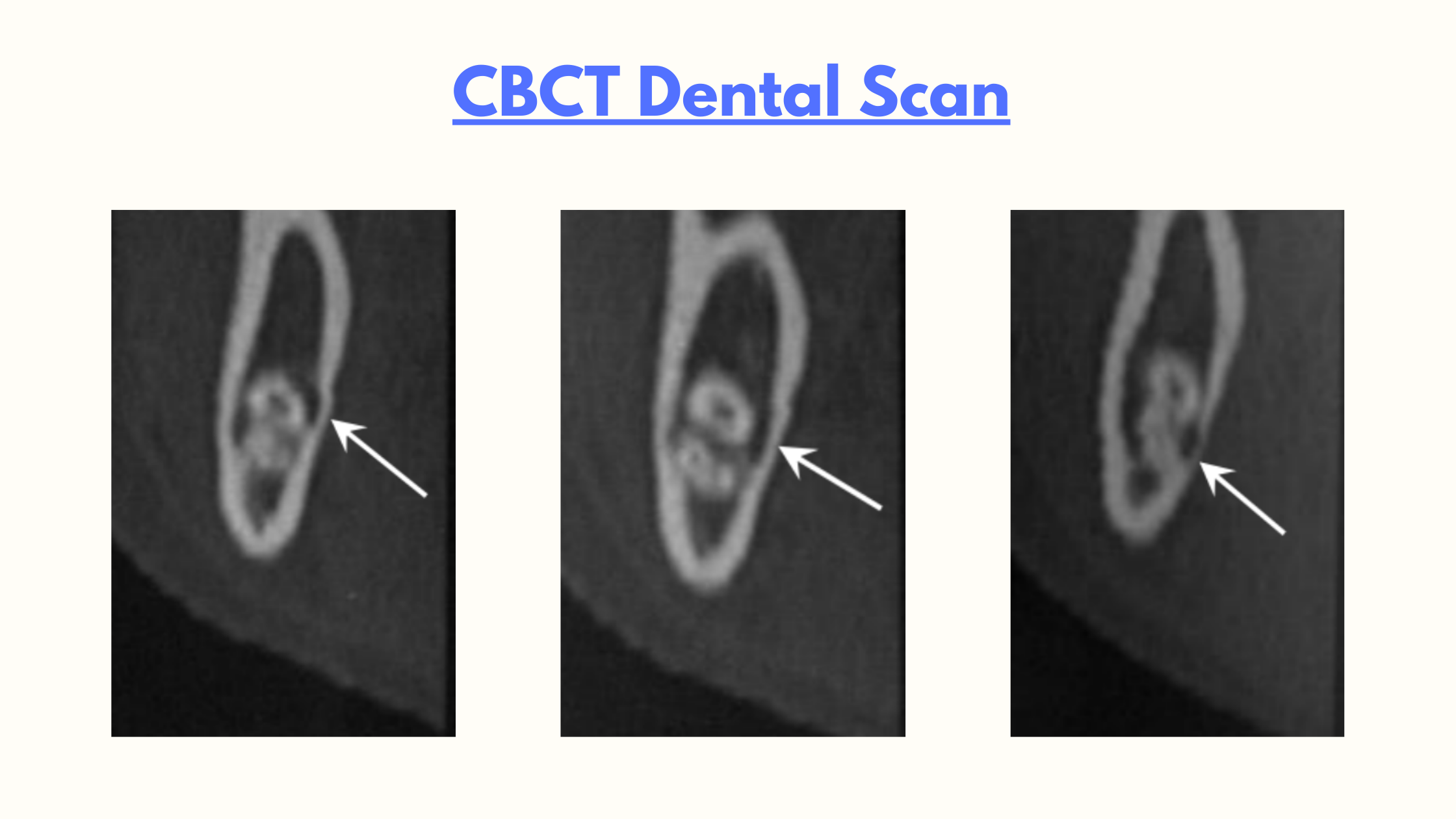
What Nerves are More Likely to be Affected?
The nerves most frequently affected during wisdom tooth removal are the inferior alveolar nerve (also called the mandibular nerve) and the lingual nerve. Both are branches of the trigeminal nerve, which is responsible for sensations in most of the face and mouth.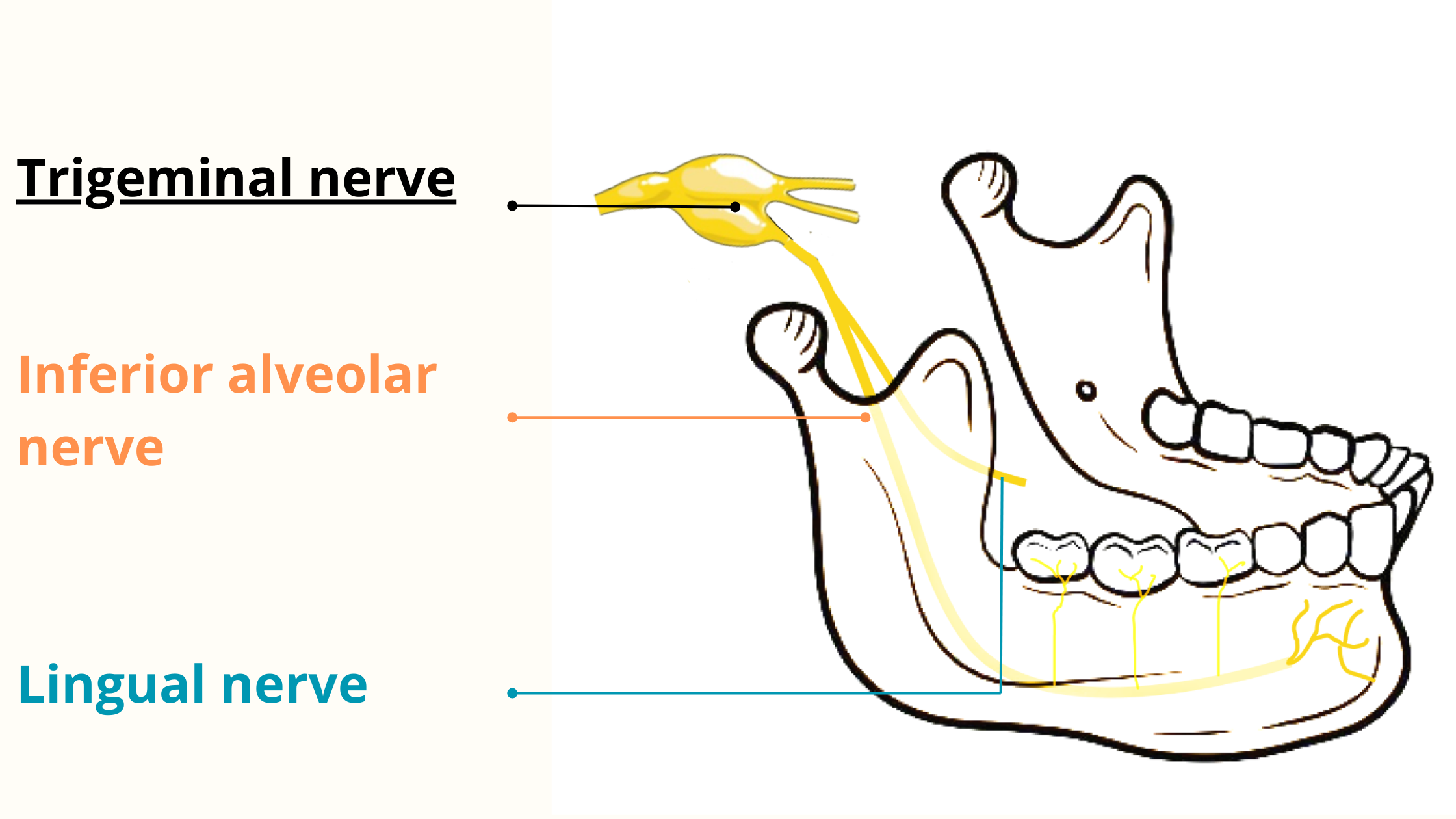
These nerves run through the lower jaw and pass very close to the wisdom teeth. In some cases, they can even be in direct contact with the tooth, which raises the risk of injury during extraction.
It’s important to note that both the lingual and mandibular nerves are sensory. They carry signals like touch, temperature, and pain to the brain, but they do not control facial movements.
That means if these nerves are injured, you might notice changes in sensitivity—such as numbness or tingling—but by no means paralysis or loss of control of your facial expressions.
What happens when the lingual nerve is damaged?
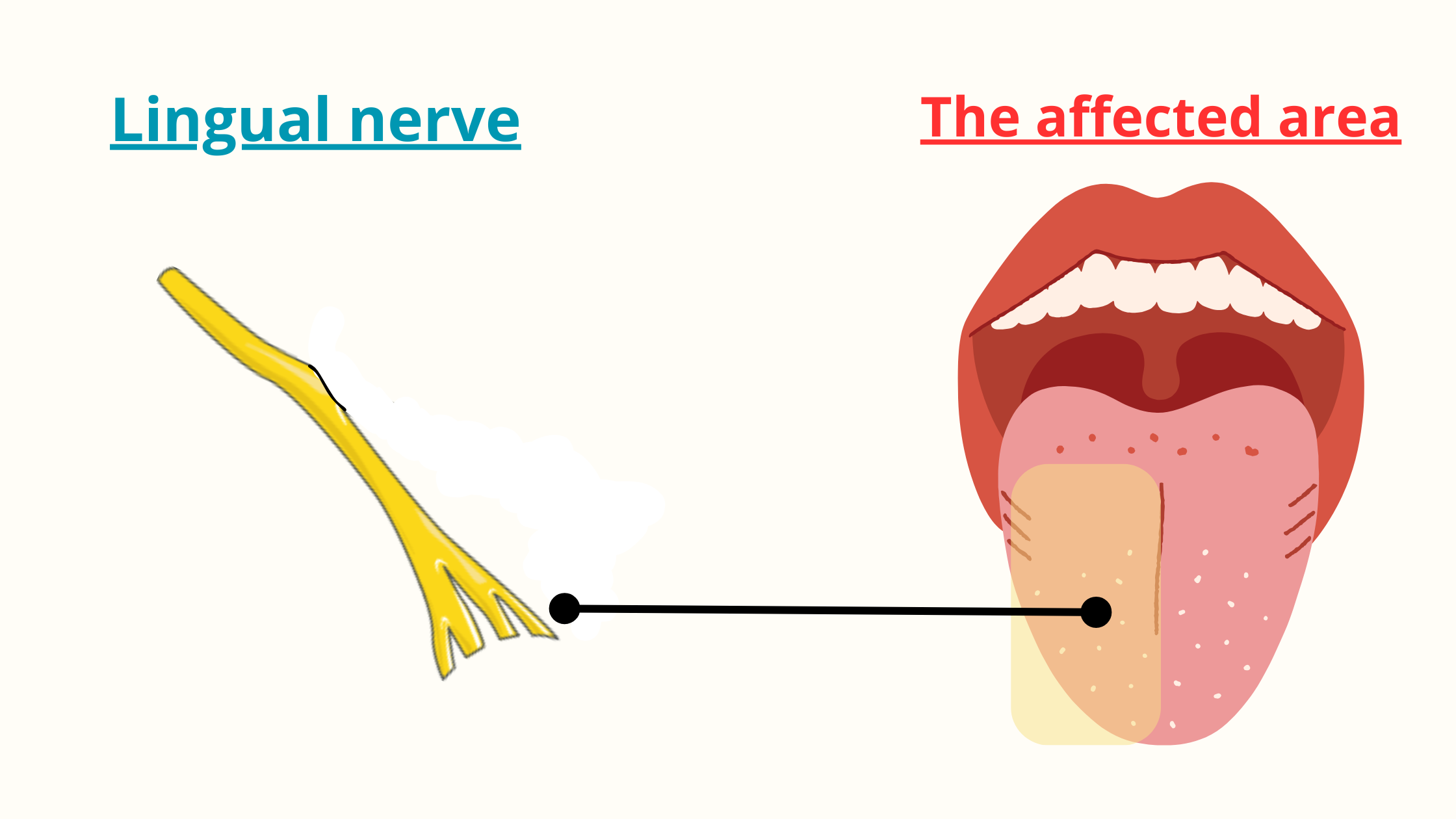
The lingual nerve provides sensation to the front two-thirds of the tongue, the floor of the mouth (under the tongue), and the gums on the inside.
If this nerve is damaged, you may experience a loss of sensation in the tongue, which can also affect your sense of taste.
Because the lingual nerve also helps control salivary glands, damage may sometimes lead to reduced saliva production and a dry mouth.
Effects of inferior alveolar nerve damage
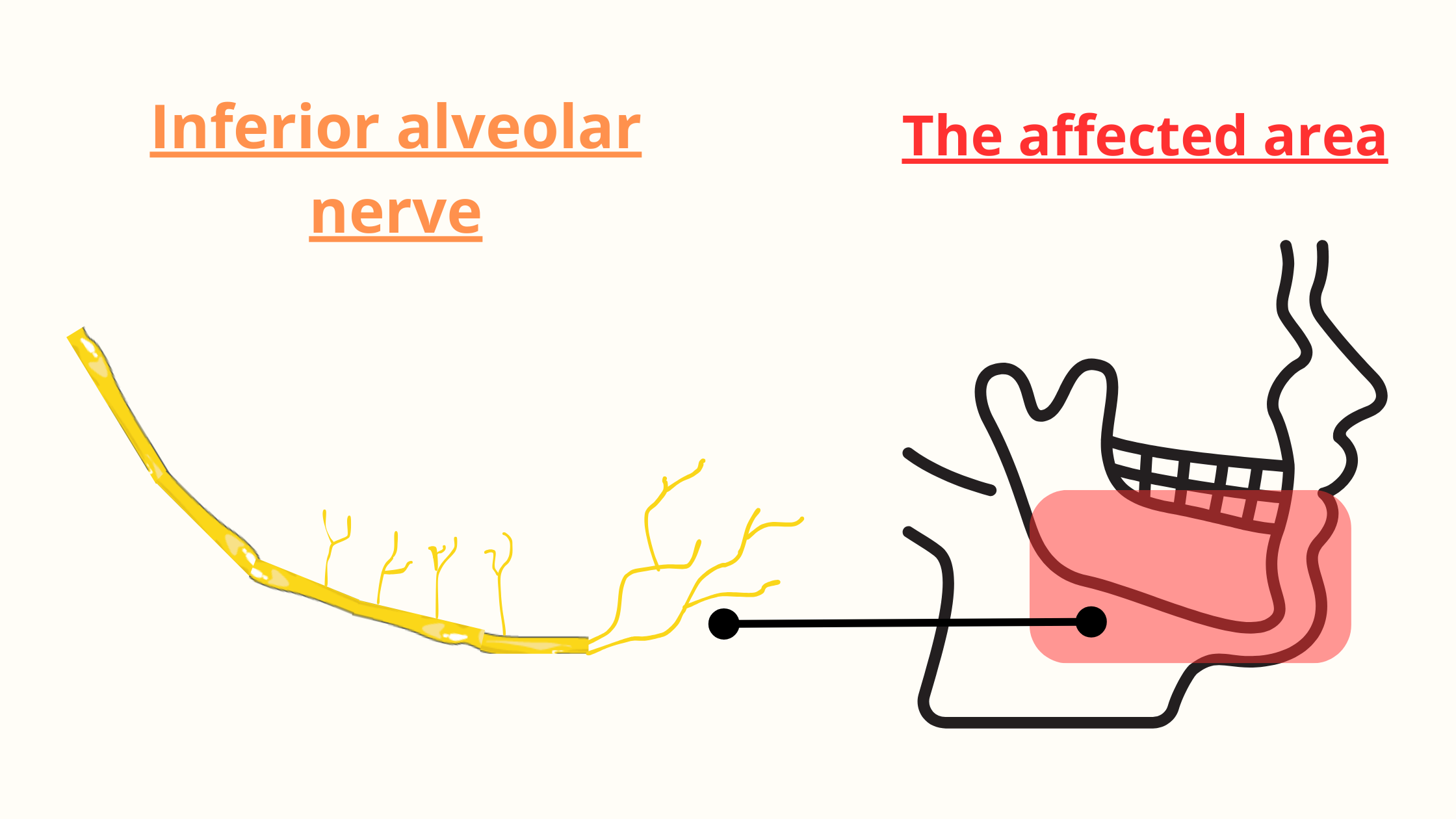
The inferior alveolar nerve provides sensation to the teeth, the front part of the gums, the lower lip, and the chin. Injury to this nerve can result in numbness in all these areas.
What type of nerve damage can occur in wisdom tooth extraction?
Nerve injuries can be classified based on their cause and severity:Based on the cause:
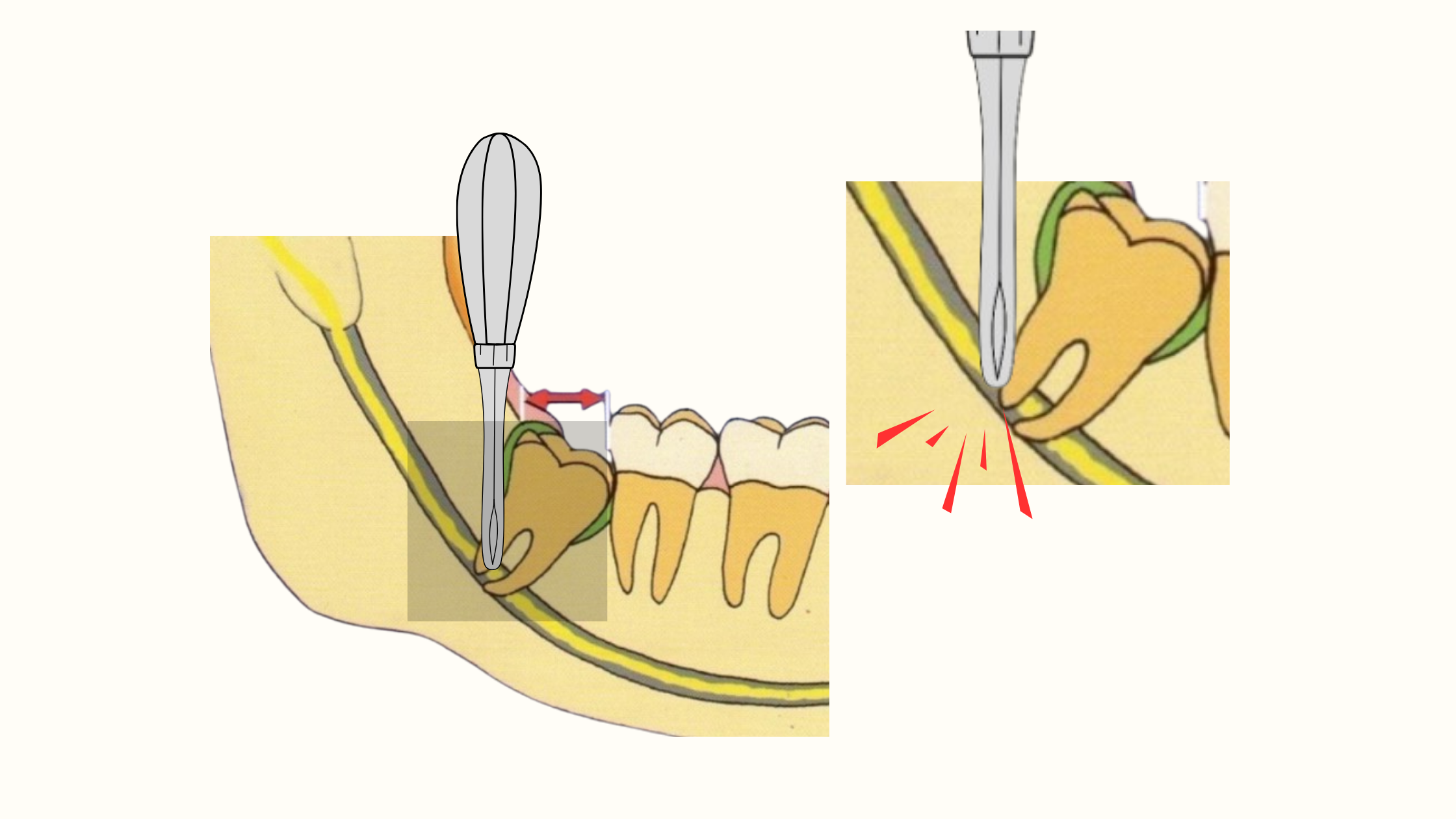
- Accidental injury caused by a sharp instrument used during extraction. The injury may be a simple irritation or, in extreme cases, a cut.
- Injury caused by the anesthetic needle. The needle used for the injection may pierce a nerve. This is usually minor and reversible.
- Nerve compression due to the post-operative swelling and bruising. Swelling after the procedure can put extra pressure on the nerve, causing tingling or numbness. These sensations usually fade quickly as the swelling goes down.
Based on the severity:
Nerve injuries during wisdom tooth removal are often minor, consisting of a mild stretch or rubbing of the nerve. This can cause temporary sensory changes, which usually improve on their own as the nerve heals.
In rare cases, the nerve may be completely severed, leading to long-lasting or even permanent changes.
However, during the first few months, it's too early to jump to conclusions. Recovery can sometimes occur months or even years later, even if the damage initially seems permanent.
There’s also a rare condition called delayed paresthesia, where abnormal sensations don’t appear immediately but show up weeks later. Like most mild nerve injuries, these symptoms are usually temporary and resolve over time.
I feel a tingling sensation after anesthesia. Is this normal?
Feeling a tingling sensation in your lower jaw right after anesthesia injection is a positive sign that the anesthesia is taking effect. This sensation should resolve within a few hours after the procedure.If the nerve is accidentally damaged by the needle, these effects can persist slightly longer.
Lost control of facial expressions on one side after anesthesia—Is it normal?
There’s also a small risk that the anesthesia injection can reach the facial nerve, which controls facial movements. This usually happens if the needle goes a little deeper than it should.
This can cause temporary facial paralysis on that side of the face. It’s usually not serious and typically resolves within a few hours.
What are the most common symptoms?
During the first week or two, it can be hard to tell normal side effects from a potential nerve injury.The only way to know for sure is to monitor your symptoms and see if they last longer than expected.
Normal side effects gradually improve over time, while nerve injuries may take longer to heal.
Keep in mind that even if symptoms seem to last forever, recovery can still occur within the first six months, and improvement may continue for up to 24 months!
Here are the most common signs to be aware of:
Sensation impairment:
This may appear as tingling and prickling sensations on the gums, lower lip, lower cheek, chin, and tongue.
Intense, radiating pain:
Others may experience intense, radiating pain, often described as a burning sensation. This pain may extend to other parts of the face and can occur periodically, lasting for hours.
Complete loss of sensation:
In cases where the nerve is completely severed, there may be total numbness in the involved area.
Disturbance of oral functions:
Nerve damage can cause difficulties with speaking and increase the risk of accidentally biting your lip or tongue.
Taste impairment and dry mouth:
The lingual nerve, which passes near the lower wisdom tooth, carries nerve fibers that control taste and saliva production. Damage to these nerves can result in problems like dry mouth, bad breath, and loss of taste, impacting oral health.
Can nerve damage lead to facial paralysis?
The nerve most likely to be damaged is mainly sensory and does not control facial movements, so an injury to it cannot cause paralysis.After having your wisdom teeth removed, it’s common to experience difficulty opening your mouth, speaking, or chewing. These side effects often appear the day after the procedure and are completely normal.
Why does this happen? Holding your mouth open for an extended period during the procedure can put extra strain on your jaw joints, muscles, and surrounding ligaments.
This strain can cause temporary soreness, stiffness, and tightness in the jaw muscles. These effects usually improve gradually on their own.
When does recovery from nerve damage usually occur?
Recovery usually occurs within the first six months after surgery. If symptoms persist beyond this period without any improvement, there is a chance that the nerve damage could be permanent and might require surgical intervention.However, studies show that recovery can continue for up to 24 months. So in many cases, a “watch and wait” approach is preferable before considering more invasive treatments.
Nerve damage treatment
Even in the worst-case scenario—where the nerve is completely severed—there are several options to support healing and regeneration.The first approach is to allow time for natural recovery. Nerves have a strong regenerative potential, so there’s a good chance of repair, especially for minor damage. This process can take some time, particularly for the inferior alveolar nerve.
If symptoms persist or the injury is severe, a surgical procedure may be considered. This intervention aims to decompress and repair the damaged nerve by reconnecting its ends, helping the severed parts fuse and regenerate properly.
Should wisdom teeth that carry a risk be left in place?
Deciding whether to remove or keep your wisdom teeth involves weighing the pros and cons of the procedure. Your dentist will explain the potential risks and benefits so you can make the best choice for your situation.If your wisdom teeth have erupted correctly and are in the right position, you may never need to have them removed.
Unfortunately, these teeth often don’t have enough space in the jaw to fit properly. This can lead to problems such as infections, cavities, cysts, and pain. In such cases, the benefits of extraction usually outweigh the risks of the procedure.
But what if a wisdom tooth must be removed but is located very close to a nerve? In these situations, careful examination with X-rays is crucial to prevent potential nerve complications.
If X-rays show that the nerve is very close to the tooth roots and injury is unavoidable, a procedure called a coronectomy can be used. This involves removing only the crown of the tooth while leaving the roots in place.
However, coronectomy isn’t suitable for every case. It has limitations, particularly when there’s an infection, a cyst, or if the tooth is badly angled.
In any case, the extraction should be done as gently and atraumatically as possible to minimize the risk of serious or permanent nerve damage. This way, even if a nerve is accidentally injured, the damage is usually minor and unlikely to cause lasting problems.
- Delayed paresthesia of inferior alveolar nerve after dental surgery: case report and related pathophysiology - PMC (nih.gov)
- Inferior Alveolar Nerve Injury after Mandibular Third Molar Extraction: a Literature Review - PMC (nih.gov)
- Inferior Alveolar Nerve Deficits and Recovery Following Surgical Removal of Impacted Mandibular Third Molars - PMC (nih.gov)
- Management and prevention of third molar surgery-related trigeminal nerve injury: time for a rethink - PMC (nih.gov)
- Lingual Nerve Injury: Surgical Anatomy and Management (oralhealthgroup.com)