Leukoplakia: More than just White Patches in the Mouth
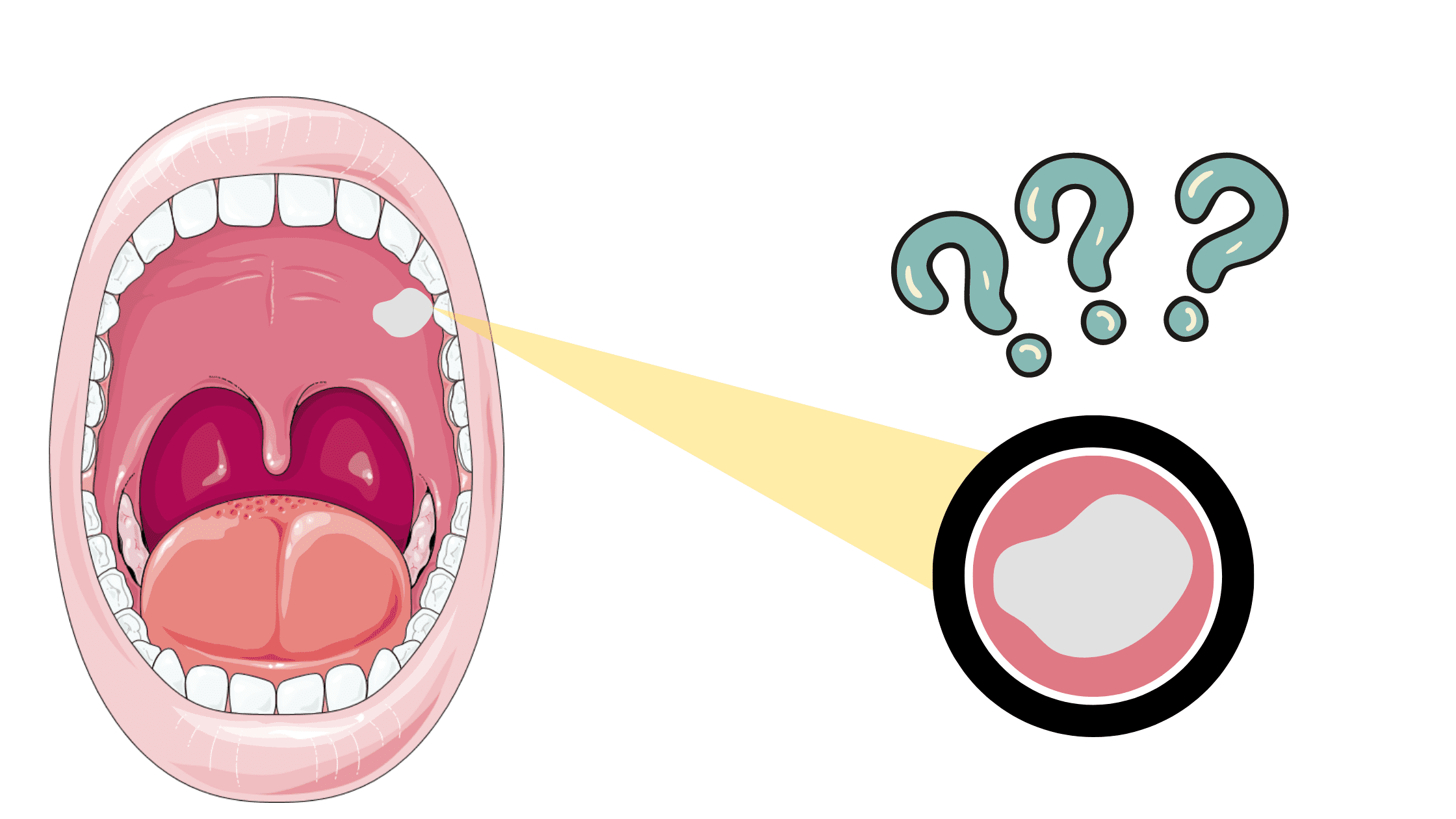 White patches in the mouth can mean many different things. They might be caused by ulcers, fungal infections, irritation or injury, or even allergies.
White patches in the mouth can mean many different things. They might be caused by ulcers, fungal infections, irritation or injury, or even allergies.
Leukoplakia is another condition that can lead to white patches anywhere in the mouth. Because these patches often look similar to those caused by other issues, a biopsy is usually needed to confirm the diagnosis.
This article is your complete guide to understanding leukoplakia—what it is, how to recognize it, the risks involved, treatment options, and how to keep it from getting worse.
In this article:
1. Understanding Leukoplakia
2. The Main Features of Leukoplakia
3. What Causes Leukoplakia?
4. Who's Most Prone to Leukoplakia?
5. Leukoplakia and Its Link to Oral Cancer:
6. Does Leukoplakia Require Treatment?
7. Preventing Leukoplakia: Some Strategies
Understanding Leukoplakia
Leukoplakia is a medical term that describes those white patches or plaques you might notice inside your mouth. "Leuco" means 'white color,' and "Plakia" refers to 'tissue changes.'These white patches can appear anywhere in the mouth—on the inside of the cheeks, tongue, lower lip, or gums. They can’t be scraped off and are not caused by something building up. Instead, they develop due to deeper changes in the mouth’s lining.
Leukoplakia happens when the mouth’s lining thickens and starts producing too much keratin—the same tough protein found in your hair and nails. This buildup of keratin is also what gives the patches their white appearance.
What Triggers Leukoplakia?
It's often the same factors that lead to oral cancer, especially tobacco use. Other irritants, like alcohol or chronic trauma, can also contribute.
While leukoplakia itself isn’t cancer and is often harmless, it can sometimes carry a precancerous potential. That’s why it’s considered a “potentially malignant oral disease.”
So, where does this cancer risk come from?
Leukoplakia can cause abnormal changes in the cells of the mouth lining — a condition known as dysplasia. And dysplasia can be an early warning sign because it sometimes progresses to cancer if left unchecked.
In dysplasia, the changes only affect the surface layer of the tissue. It’s not cancer yet, and it can be fully cured once the cause is treated.
The Main Features of Leukoplakia
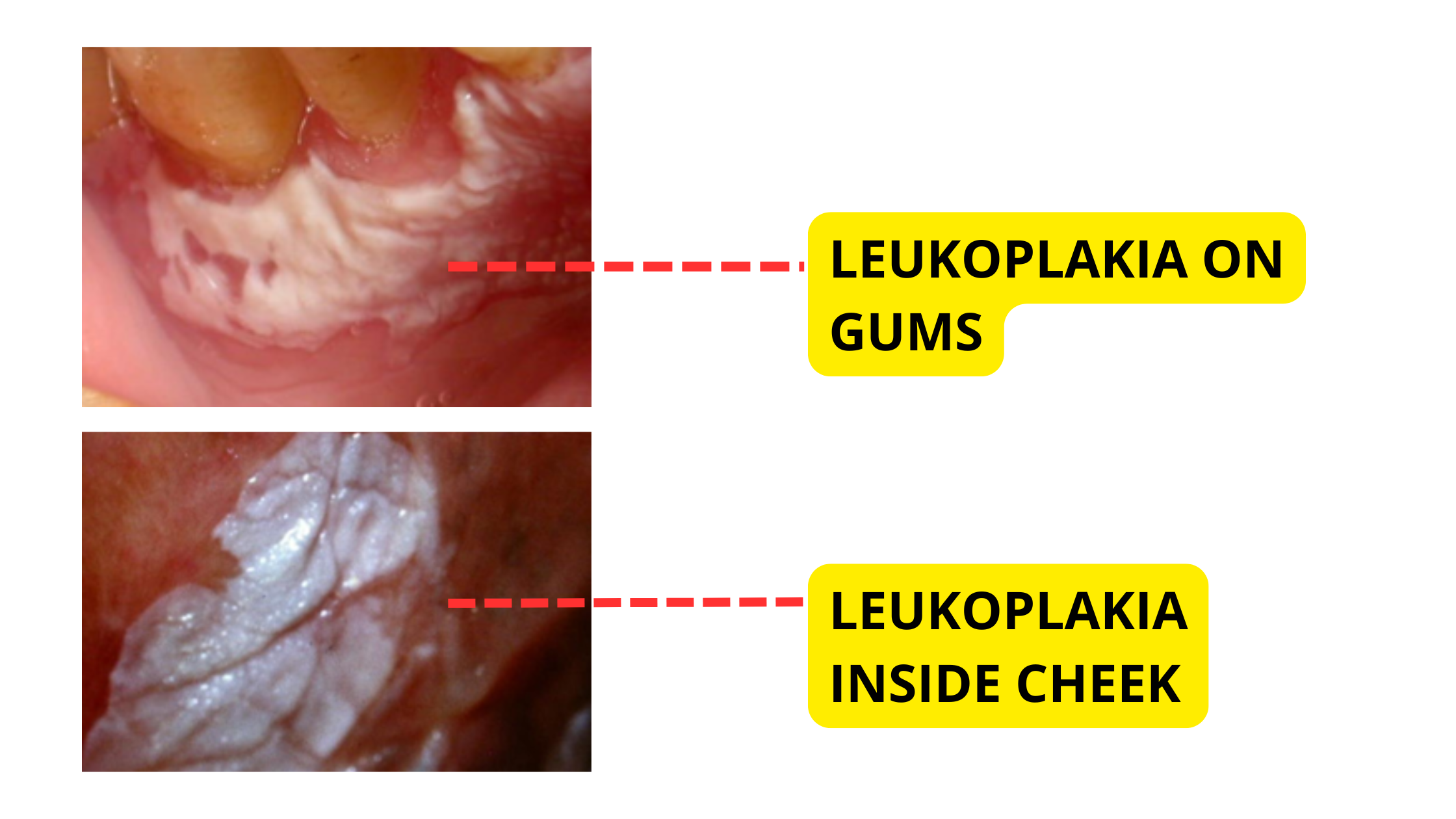 Leukoplakia can look and develop differently from person to person, but these are the main features to be aware of:
Leukoplakia can look and develop differently from person to person, but these are the main features to be aware of:
1. The Primary Feature:
White patche inside your mouth, which can be flat or slightly raised. You can't scrape it off. It’s deeply embedded within the lining of the mouth.
2. Size, Shape, and More:
- Size: The white patches can range from just a few millimeters to larger, more widespread areas.
- Shape: The borders of these patches are usually irregular and uneven.
- Texture: Lesions can be smooth and thin—or rough, thick, and grooved.
- Color: Leukoplakia plaques are typically grayish-white. They may also appear with red spots or small ulcers. In smokers or heavy coffee drinkers, the patch might look brownish-yellow.
- Symptoms: Leukoplakia is usually painless, but thicker patches can become easily irritated or injured while chewing, leading to discomfort.
What Causes Leukoplakia?
Leukoplakia has several potential causes, but the best-known trigger is tobacco in its various uses.Leukoplakia can sometimes occur without any clear reason, which we call Idiopathic Leukoplakia. But, most of the time, there's something specific constantly irritating the mouth, such as infections, alcohol, smoking, or chronic irritation.
1. Tobacco: The Main Culprit
Tobacco, whether smoked or smokeless, is the major cause of leukoplakia. Smokers run about 4 to 6 times more risks than non-smokers.
The reason is that tobacco and its by-products actually have a toxic effect on your mouth cells. The heat from smoking adds even more damage to the tissues. Over time, these toxic effects can add up, increasing the risk of precancerous and even cancerous changes.
2. Other Risk Factors
Aside from tobacco, there are other risk factors that can contribute to leukoplakia, including:
- Alcohol: When combined with tobacco, alcohol drastically raises the risk of leukoplakia, as well as oral and throat cancer. If you use both, it's even more important to keep a close watch on these lesions.
- Chronic Irritation: Constant small injuries or frictions to the lining of your mouth can, over time, affect cell function and cause local changes, like ulcers, white patches, and lumps.
- Nutritional Deficiency: Certain vitamin and mineral deficiencies can affect your mouth in different ways.
A lack of iron may lead to tongue inflammation and soreness.
Low levels of B-complex vitamins are often linked to repeated mouth ulcers.
And if you’re low on vitamin A, your body might produce too much keratin—the same protein found in leukoplakia patches. - Mouth Infections: Certain infections, such as oral thrush (caused by the yeast Candida albicans) or Human Papillomavirus infection (HPV), can affect the lining of your mouth and cause changes similar to leukoplakia.
Who's Most Prone to Leukoplakia?
Leukoplakia affects about 1.5% to 4.1% of people. It’s more common in middle-aged and older adults, mostly appearing in people in their 40s, 50s, and 60s. It’s rare before age 30, making up only about 5% of cases.Men are more prone to develop leukoplakia than women—mainly because smoking is more common among men. However, as more women today are taking up smoking, this gap is beginning to narrow.
There is a specific type called hairy leukoplakia. This rare form looks like tiny white hairs, usually found on the sides of the tongue. It’s most common in people with weakened immune systems, especially those who are HIV-positive, have had an organ transplant, or take long-term corticosteroids.
Leukoplakia and Its Link to Oral Cancer:
Leukoplakia is often a harmless, benign condition that poses no threat. However, as we've seen, lesions with dysplasia carry a high risk of malignant transformation.About 1% to 30% of leukoplakia lesions show dysplasia (precancerous changes). And 11% to 36% of dysplastic changes can eventually develop into oral cancer.
There's no way to tell from appearance whether the lesion is dysplastic, cancerous, or benign. So, even if the risk seems low, never ignore persistent white spots in your mouth and have them checked by your dentist or doctor as soon as possible.
If leukoplakia is suspected, a biopsy might be needed for an accurate diagnosis and to rule out other similar conditions.
As with any precancerous condition, removing risk factors—like quitting smoking or eliminating sources of irritation—can prevent the lesions from getting worse and reduce the risk of cancer.
If leukoplakia does develop into cancer, it's called squamous cell carcinoma, the most common form of oral malignancy.
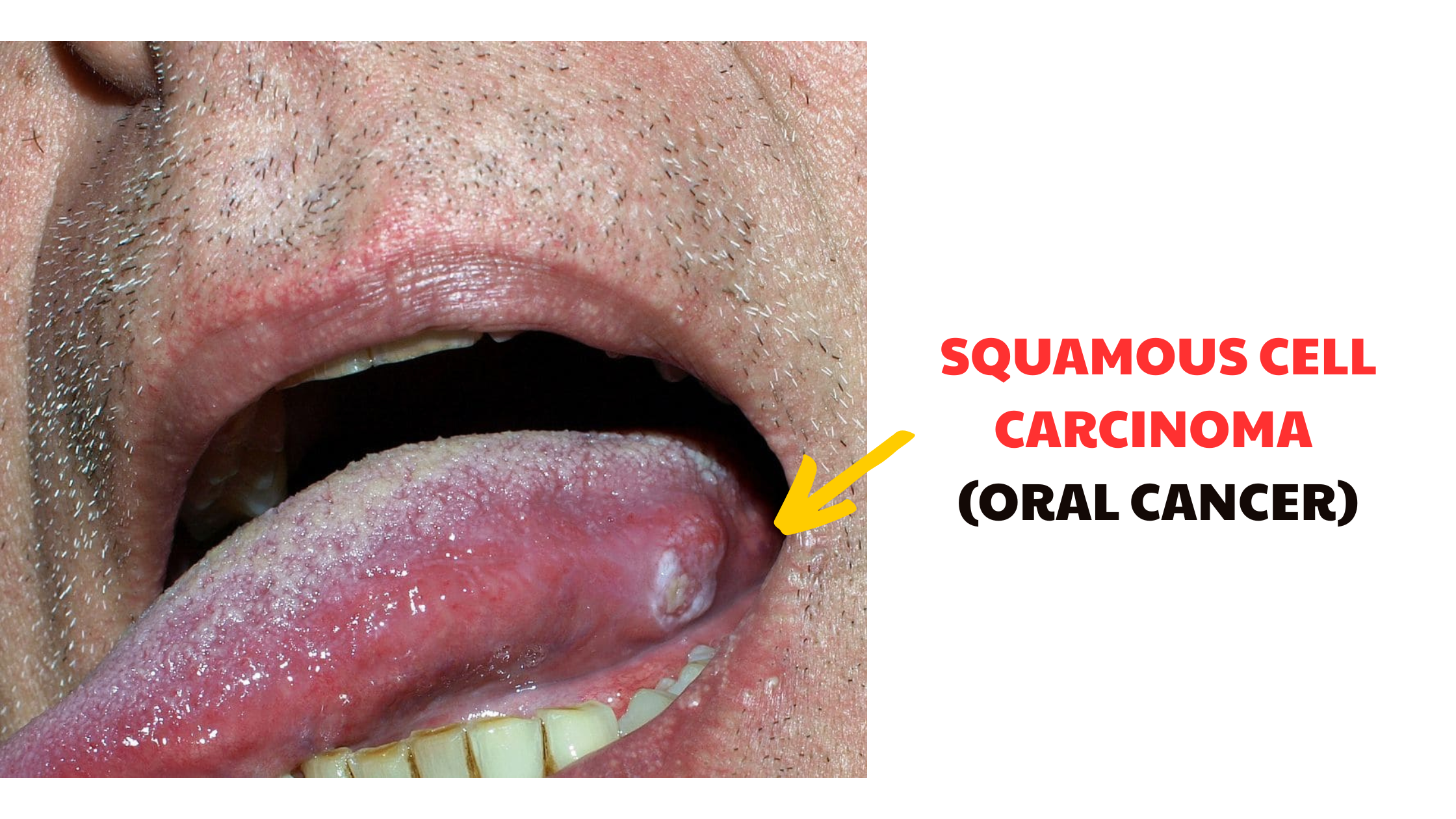
What factors increase the risk of malignant transformation?
- Location: The floor of the mouth (under your tongue) holds a higher risk, while patches on the roof of your mouth or gums have a lower risk.
- Time and Risk Factors: The longer your mouth is exposed to risk factors like smoking, the greater the potential for cancer.
- Size and Shape: Larger and more irregular patches usually pose a higher risk.
- Nature of the Lesion: Only a microscopic examination can reveal the true precancerous nature of the disease. If cells appear abnormal (dysplastic), the precancerous potential is there.
- Age: Overall, oral cancer risk increases with age.
Does Leukoplakia Require Treatment?
The answer depends on the biopsy results. A biopsy is a simple procedure where a small tissue sample is taken from the affected area and examined under a microscope.This helps confirm if the patch is truly leukoplakia and whether there’s any risk of it becoming cancerous in the future.
- If the cells look normal (no dysplasia), you might not need any treatment. In this case, removing risk factors like quitting smoking and having regular check-ups every six months may be enough.
- If the cells appear suspicious or show signs of precancerous changes, surgical removal of the patches is usually recommended to eliminate the risk of cancer.
Preventing Leukoplakia: Some Strategies
Some strategies to prevent leukoplakia from worsening or recurring include:- Remove the Risks: Get rid of all the risk factors that may be involved in leukoplakia. Stop smoking and limit alcohol consumption. Treat any mouth infection and address any nutritional deficiencies.
- Stop any Source of Irritation: If something is causing constant irritation in your mouth, it needs to be addressed. It could be a dental crown that doesn’t fit properly or a sharp tooth edge that’s constantly rubbing against your cheek or tongue. Even habits like teeth clenching and grinding should be checked.
- Protect Yourself: Because some STDs may contribute to the condition, always protect yourself during high-risk sexual activities.
- Follow-up: Regular check-ups with your dentist or doctor are key. These visits may include biopsies to watch for any changes or progression.
- Effect of tobacco in human oral leukoplakia: a cytomorphometric analysis - PMC (nih.gov)
- Idiopathic Leukoplakia- Report of a Rare Case and Review - PMC (nih.gov)
- Oral leukoplakia - UpToDate
- Relationship of Vitamin A and Oral Leukoplakia | JAMA Dermatology | JAMA Network
- A Color Handbook of Oral Medicine De Richard C. K. Jordan, Michael A. O. Lewis
- Essential Of Oral Pathology - Book by Swapan Kumar Purkait