Gum Ulcer: Every Potential Cause Explained
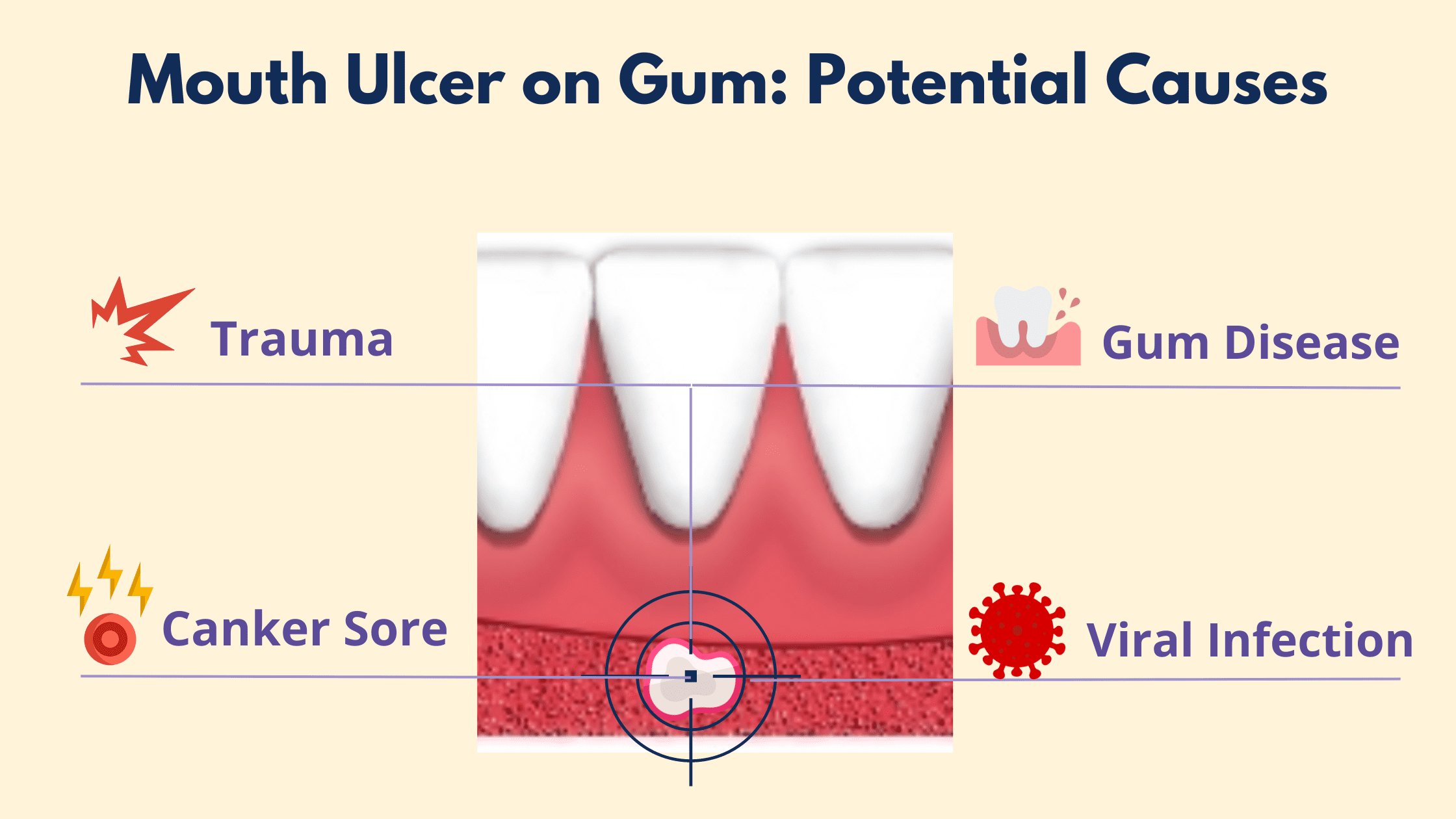 Have you ever looked in the mirror and noticed a sudden, painful white or red spot on your gums? This might be a gum ulcer.
Have you ever looked in the mirror and noticed a sudden, painful white or red spot on your gums? This might be a gum ulcer.
While gum ulcers are not very common, they can still occur due to various reasons. These can range from infections and allergies to injuries or even a simple canker sore. Understanding the cause is key to taking the right steps for treatment.
In this article, we'll explore all the potential causes of gum ulcers, how to identify them, and most importantly, how to ensure a smooth and speedy recovery.
1. Is it a painful single ulcer? It's probably a Canker Sore.
2. Traumatic Ulcer: When Accidents Hurt Your Gums
3. Multiple Gum Ulcers due to Viral Infection
4. Necrotizing Ulcerative Gingivitis
5. When Should a Gum Ulcer Raise Concern?
6. Do's When Having a Mouth Ulcer
7. Don'ts When Having a Mouth Ulcer
1. Is it a painful single ulcer? It's probably a Canker Sore.
If you've suddenly noticed a painful single sore in your mouth and can't figure out where it came from, there's a good chance it's a canker sore.
Canker sores are common, and most people will get at least one in their lifetime. If this is your first time, you're lucky—some people get them several times a year.
They can show up anywhere inside your mouth, like on the inner lips, cheeks, under the tongue, and the roof of your mouth.
Canker sores rarely appear on the gums because they’re protected by a tough protective layer called keratin. Keratin is the same protein that makes up your hair and nails.
When canker sores do affect the gums, it’s usually on the part without keratin, near the base and away from your gum line.

Symptoms
The symptoms of mouth ulcers are quite obvious. They can show up as a single sore or in small groups of up to five. They're surrounded by a red circle and have a yellowish-white center. They are usually round or oval in shape and measure only a few millimeters.
Causes
The exact cause of canker sores is still a bit of a mystery. However, there are a few likely factors that might contribute:
- Genetics: If others in your family have had these, you might be more prone to them.
- Nutrition: Some nutritional deficiencies can increase your risk, especially if you lack vitamins B12 and B9, iron, and zinc.
- Stress: Stress can affect your mouth just like the rest of your body. If you've been through a difficult period (work overload or illness), mouth ulcers may appear.
- Hormones: Hormonal changes can sometimes trigger these sores.
- Allergies: Your mouth may be too sensitive to certain foods like seafood, chocolate, tomatoes, nuts, and strawberries.
The 4 Stages of Canker Sores
Canker sores go through four stages as they develop:
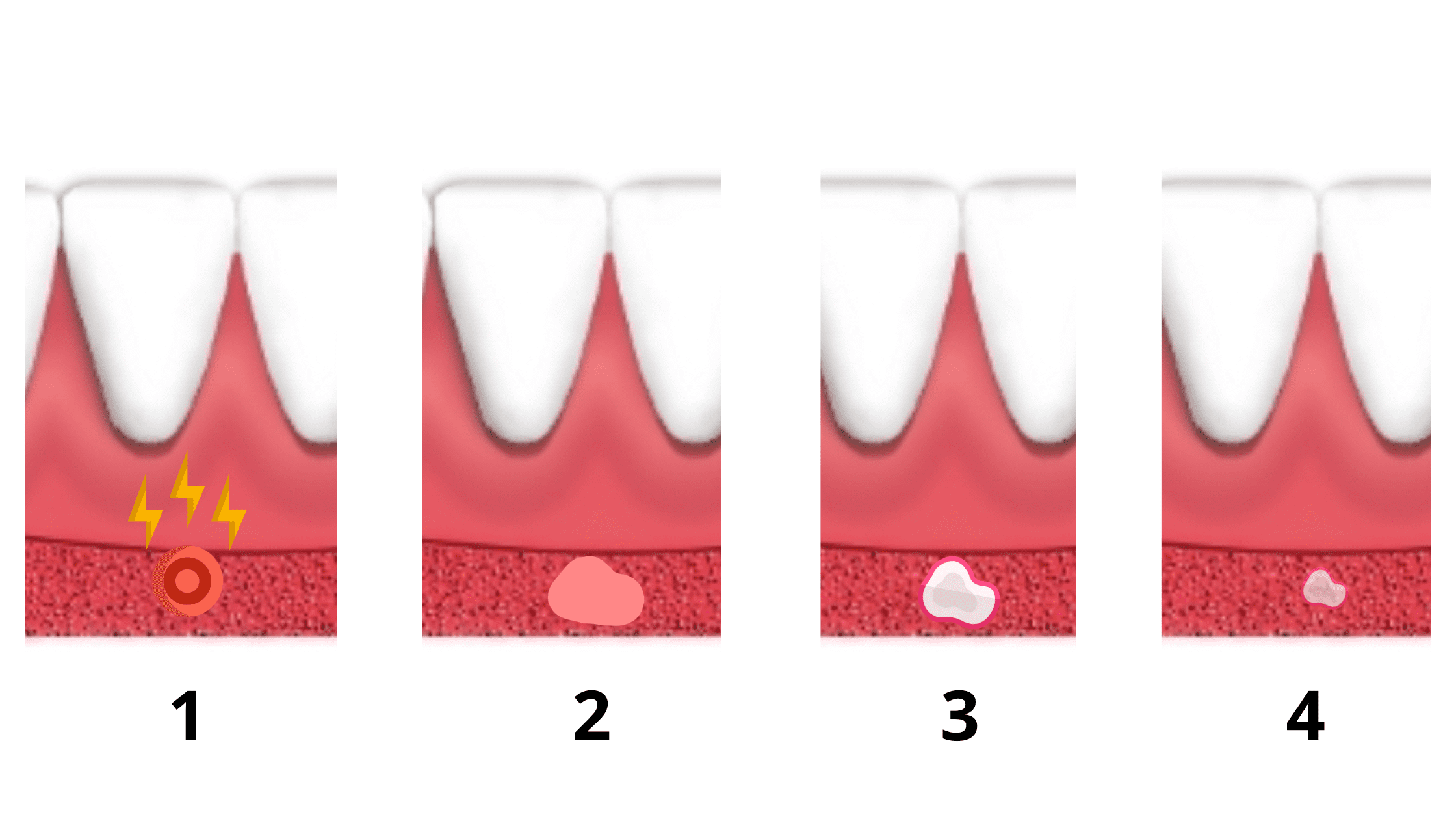
- The Prodromal Stage: This early phase lasts 24 hours. You might start feeling a tingling or burning sensation in the area where the sore is about to appear.
- The Macule Stage: From 18 hours to 3 days, you'll see a red or pink spot in the area.
- The Ulcer Stage: You'll notice a shallow, round ulcer with a whitish or yellowish coating. This is when the pain can be at its peak.
- The Healing Stage: Canker sores eventually heal on their own. The sore gradually shrinks and then disappears altogether.
How are Canker Sores Treated?
Unfortunately, there's no magic treatment to make canker sores disappear instantly. The good news is they usually heal on their own within 8 to 10 days and typically don’t leave any scars.
What you can do is speed up the healing process, manage the pain, and prevent infections or future flare-ups. There are several solutions that can help:
- Numbing Agents: These can provide instant relief by numbing the sore, making it less painful. One over-the-counter numbing product is Orajel.
- Mouthrinses: These help keep the area clean, reducing the risk of infection and promoting healing. You can rinse your mouth several times a day with salt water and baking soda, or consider using an over-the-counter peroxide-based mouthwash.
- Topical Corticosteroid Treatment: These are usually needed for severe cases. If your sore is large and very painful, your dentist may prescribe a product that includes cortocisteroids.
Prevent Canker Sores
Knowing what triggers your flare-ups will help you prevent or reduce episodes. Here are a few things to consider:
- Stress: If you believe stress is causing the issue, it's a good idea to find ways to relax and engage in activities that can help you handle it better.
- Food sensitivity: Think back to what you ate about three days before the sore popped up. Certain foods could be the culprit.
- Nutritional Deficiencies: If you're lacking certain vitamins and minerals in your diet, addressing these deficiencies can help prevent future outbreaks. B12, B9 and iron supplements have been shown to minimize recurrence.
- Avoid Injury or Trauma: Remove any sources of injury or trauma in your mouth. For example, if your teeth have sharp edges, they can rub against the lining of your mouth and cause ulcers.
- Oral Hygiene: Keep your mouth clean and healthy by practicing consistent oral hygiene and treating cavities, gum disease, and existing infections. A healthy mouth is more resistant to canker sores and many other dental problems.
2. Traumatic Ulcer (caused by injury to the gum)
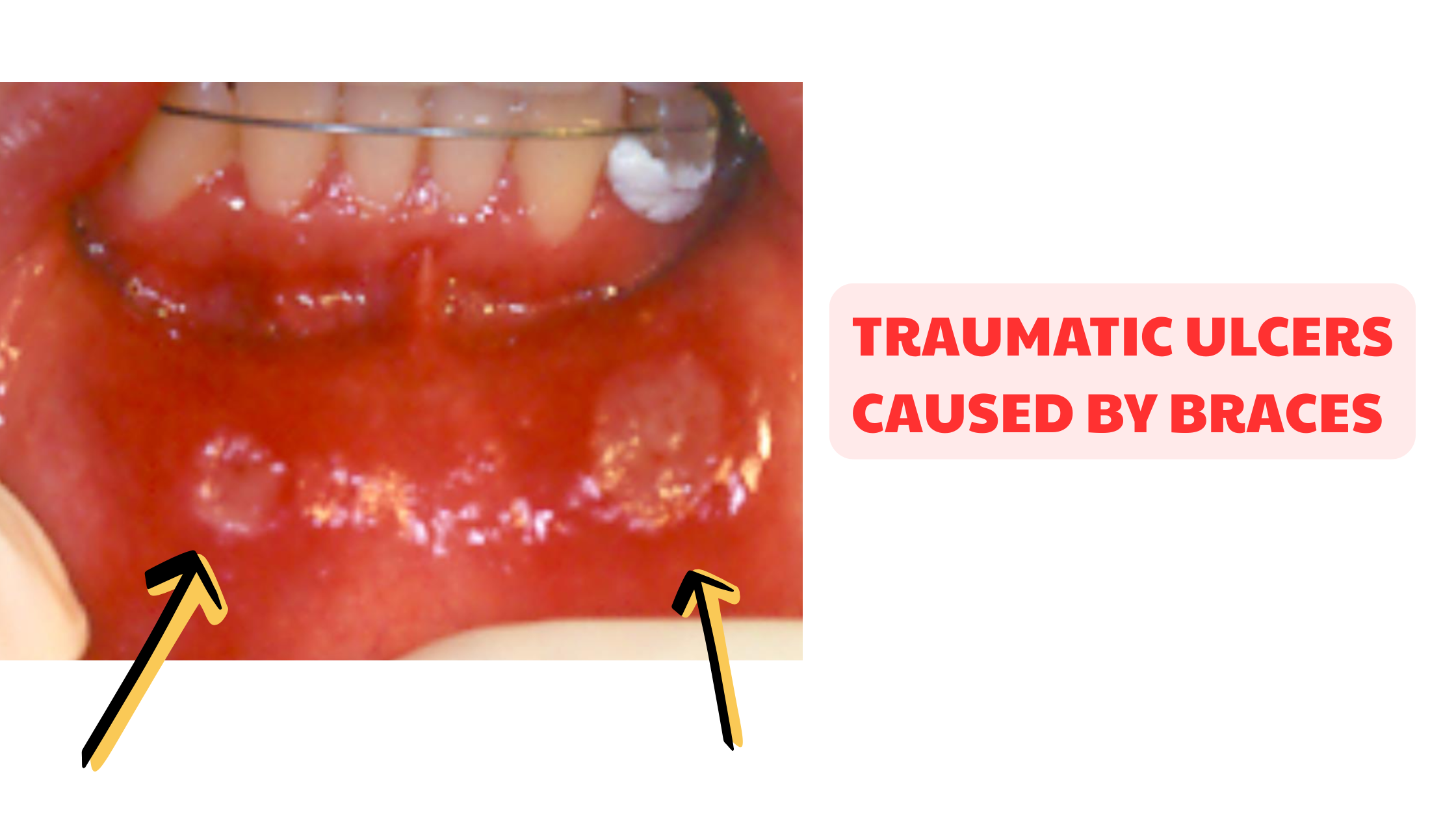
If you brush your teeth too aggressively, use a harsh mouthwash or burn your mouth with something too hot or acidic, a type of sores called traumatic ulcers can appear.
They can appear anywhere in the mouth, exactly where the injury took place.
Traumatic ulcers usually show up as whitish or yellowish spots, without the red border often seen in canker sores.
The shape of traumatic ulcers is uneven and less defined than that of canker sores. They tend to be irregular and larger, depending on the severity of the injury.
Treatment of Traumatic Ulcer on the Gum
Traumatic ulcers always heal on their own once the cause of the injury is removed.
So the key is to identify and remove any sources of irritation. Once this is taken care of, these ulcers usually heal naturally within 8 to 10 days.
Your dentist may recommend using a topical numbing product or mouthwash for relief.
3. Multiple Gum Ulcers due to Viral Infection
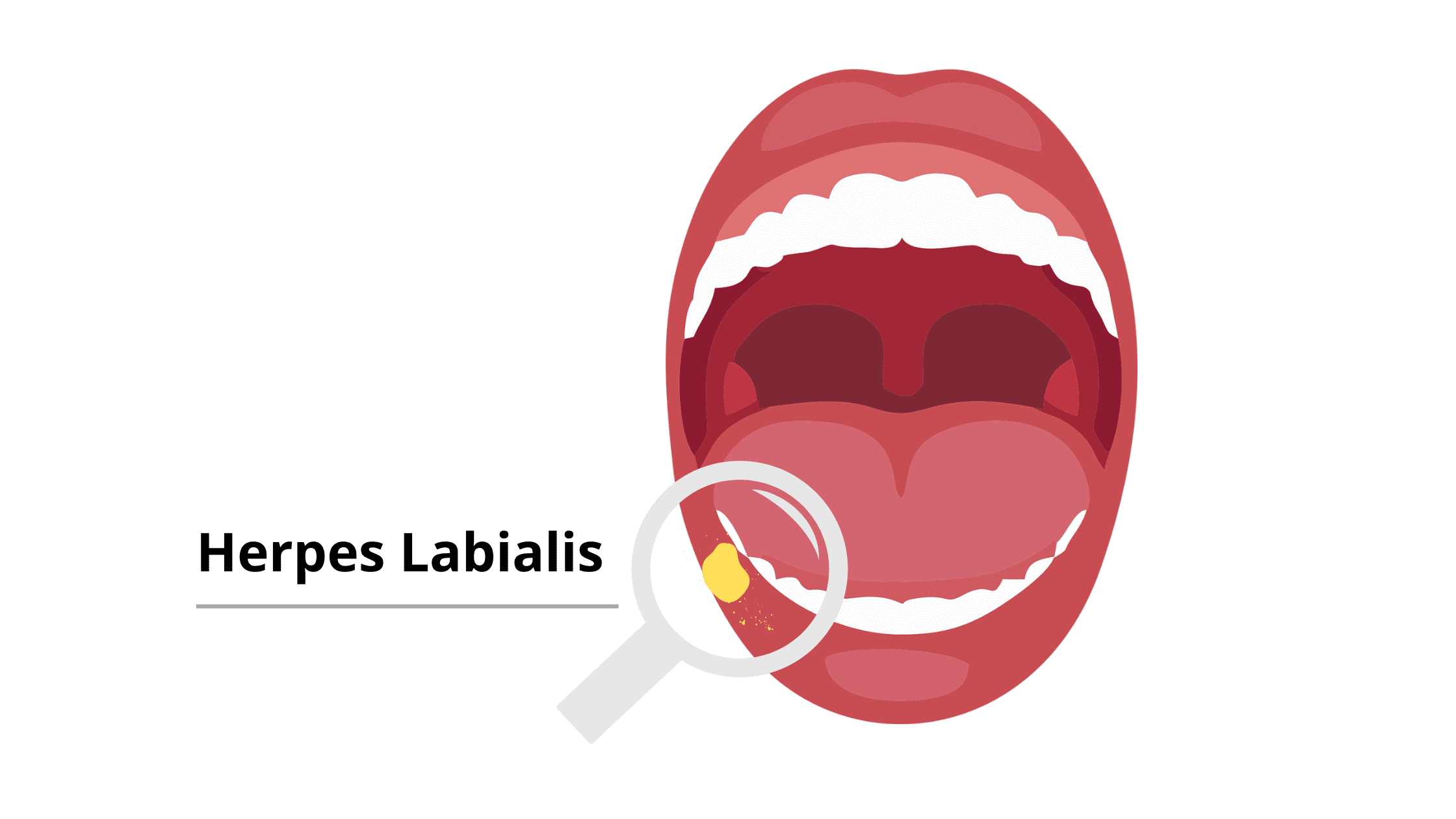
The most common viral infection affecting the mouth is oral herpes. It causes multiple sores to appear at once, commonly known as cold sores or fever blisters.
These sores often appear on the lower lip, but any part of the mouth can be affected, including the gums (as shown below).
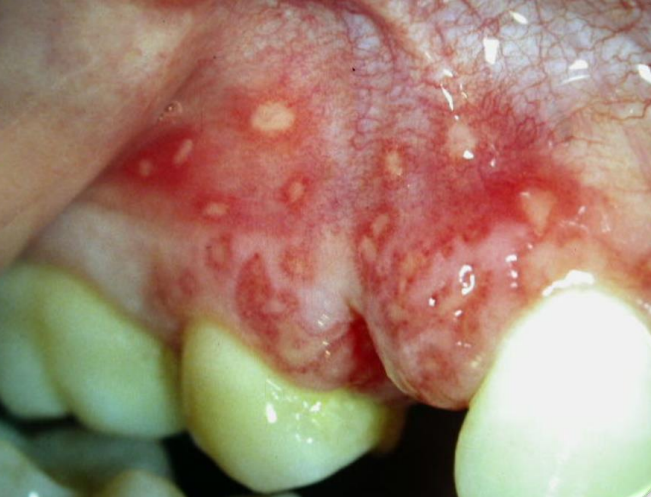
Picture of Oral Herpes Infection On Gums
Roughly 67% of people under 50 worldwide carry the herpes simplex virus type 1 (HSV-1), which is the culprit behind oral herpes sores. Typically, the virus stays dormant and doesn’t cause any symptoms.
However, the virus can reawaken at any time under certain conditions, like stress, fever, a common cold, or even trauma to the mouth.
Cold sores usually start with an itchy or burning sensation, followed a day or two later by clusters of fluid-filled blisters. These blisters eventually break open, leaving behind small, painful ulcers.
Aside from oral herpes, many other viral infections can show up as mouth ulcers. The rarest and most severe is HIV infection. People with HIV often experience multiple outbreaks, and the sores are usually larger, deeper, and more painful than in healthy individuals. They also heal more slowly and may leave scars behind.
How to Manage Viral Infections in the Mouth
Mouth ulcers caused by viral infections heal once the infection has cleared up. For example, cold sores from herpes infection typically heal in 5 to 10 days as the body fights off the virus.To speed up the healing process, your dentist or doctor may recommend:
- Topical antiviral medication
- Using an antiseptic mouthwash
- Following a soft diet
- Topical numbing gels or creams
4. Necrotizing Ulcerative Gingivitis
Necrotizing ulcerative gingivitis (NUG) is a severe form of gum disease that requires immediate attention due to its aggressive and rapid nature. One of its telltale signs is the appearance of ulcers in the triangular area of the gums, between the teeth.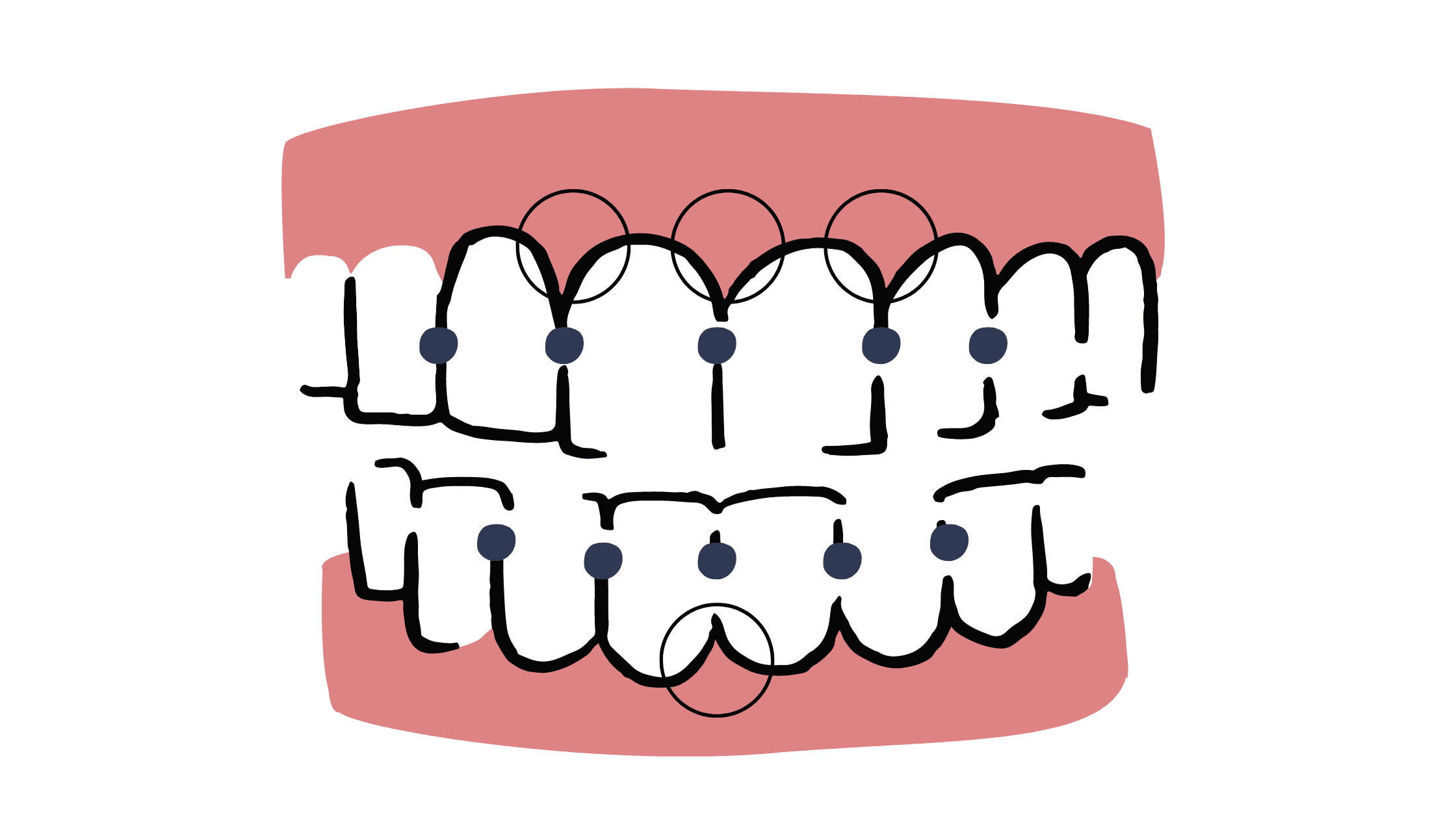
The gums between the teeth become ulcerated and covered with a whitish-grey layer, which is a sign of necrosis (tissue death).
Fortunately, necrotizing ulcerative gingivitis (NUG) is rare compared to other forms of gum disease. It mainly affects young people with weakened immune systems. Common risk factors include:
- Inadequate oral hygiene
- Stress
- HIV infection
- Tobacco use
- Malnutrition
Once NUG has set in, it often causes intense pain, bad breath, and bleeding gums. Some people may also have fever, fatigue, and swollen lymph nodes. Daily activities like eating, swallowing, and speaking can become difficult.
Without treatment, the infection can continue to destroy gum tissue and lead to extensive damage.
Treating Necrotizing Ulcerative Gingivitis
Prompt treatment is key to reverse the damage before it's too late to recover lost gum tissue.
- Professional Cleaning: It’s the only way to stop the condition from causing further damage. Since it’s often difficult to thoroughly clean painful gums at home, your dentist can remove dead tissue, debris, and bacteria—creating the right conditions for healing.
- Oral Hygiene: Consistent oral hygiene is key to keeping harmful bacteria in check. It may be difficult at first because of the pain, so start gently with a soft toothbrush and mouth rinses.
- Antibiotics if Needed: In severe cases, your dentist may prescribe antibiotics to clear the infection.
- Lifestyle Changes: If you’re at risk for this severe form of gum disease, making a few changes by addressing certain risk factors can help. This may include quitting smoking, managing stress, improving your oral hygiene, eating a healthier diet, and taking supplements if needed.
When Should a Gum Ulcer Raise Concern?
In most cases, an ulcer on your gums or anywhere else in your mouth should not be a cause for concern. Usually, it's harmless and benign and tends to resolve on its own.However, there are certain warning signs that even the healthiest individuals should never ignore.
Even if the chances of something serious are low, it’s always worth getting checked by a professional if you notice:
- An ulcer that isn’t healing or improving after 2 weeks
- An ulcer that keeps getting worse instead of healing
- A firm, hard ulcer when touched
- Irregular or protruding edges around the ulcer
- An ulcer that looks aggressive or damages nearby tissues
- Unexplained bleeding
- Persistent red or white patches in the mouth
These can sometimes be signs of oral cancer, though they may also indicate other benign conditions.
When an ulcer persists unusually long, the only way to know for sure is with a biopsy to rule out serious conditions.
How likely is a persistent gum ulcer to be cancer?
The gums are not the most typical site for oral cancer. It’s even less likely if the sore is painful (cancer rarely causes pain in its early stages).
Oral cancer more often starts in other areas, especially the sides of the tongue, the lips, or the floor of the mouth.
Still, even though the gums are more protected, it's not a reason to ignore persistent, long-lasting symptoms.
Below are some Do’s and Don’ts to help you manage discomfort while your ulcer heals.
Do's When Having a Mouth Ulcer
- Maintain Good Oral Hygiene: Keep your mouth clean by gently brushing your teeth and using a soft toothbrush.
- Rinse with Salt Water: This will help soothe the area and promote healing.
- Choose Soft Foods: Stick to a gentle, easy-to-eat diet.
- Over-the-Counter Solutions: Many numbing gels, antiseptic mouthwashes, or creams are available that can help bring relief.
- Stay Hydrated: This will help keep your mouth moist and prevent dry mouth, which can cause additional discomfort.
Don'ts When Having a Mouth Ulcer
- Avoid Irritating Foods: Steer clear of spicy, acidic, and rough-textured foods that can worsen the pain.
- Limit or Quit Smoking: Tobacco smoke contains hundreds of harmful chemicals that can damage not only your throat and lungs but also your mouth, since the smoke touches your mouth first. Try to cut down on smoking — or even better, quit completely.
- Don't Use Harsh Mouthwashes: Avoid using strong mouthwashes that can cause further irritation. Opt for milder, alcohol-free options.
- Leave the Sore Alone: Don't poke or touch the ulcer with your fingers or tongue. This can lead to further discomfort.
- Don't Ignore Persistent Symptoms: If your ulcer doesn't improve or worsens after a couple of weeks, don't ignore it. Seek professional help to rule out any serious concerns.