Toothache Without Cavity? Discover the 5 Most Common Causes
 Pain in the face and mouth is so common , affecting around 21.7% of people in the U.S. alone!
Pain in the face and mouth is so common , affecting around 21.7% of people in the U.S. alone!
Toothache is often the main culprit, and in most cases, it’s linked to cavities or tooth decay.
But cavities aren’t the only reason your tooth might hurt. Sometimes, the pain feels just like a cavity, even when there’s no visible hole or damage.
In this post, we’ll explore the most common reasons you might have tooth pain without any obvious signs of a cavity.
In this article:
1. Why Tooth Pain Isn’t Always What It Seems
2. Other Than Cavities, What May Be Causing Tooth Pain? (5 Potential Reasons)
- Gum Disease
- Dental Wear
- Tooth Trauma
- Excessive Biting Forces (Occlusal Trauma)
- Tooth Pain That Doesn’t Come from the Tooth Itself (Referred Pain)
3. Should You See Your Dentist?
Why Tooth Pain Isn’t Always What It Seems
Before we dive into the causes of tooth pain without cavities, it’s important to understand just how complex pain in the mouth and face can be.
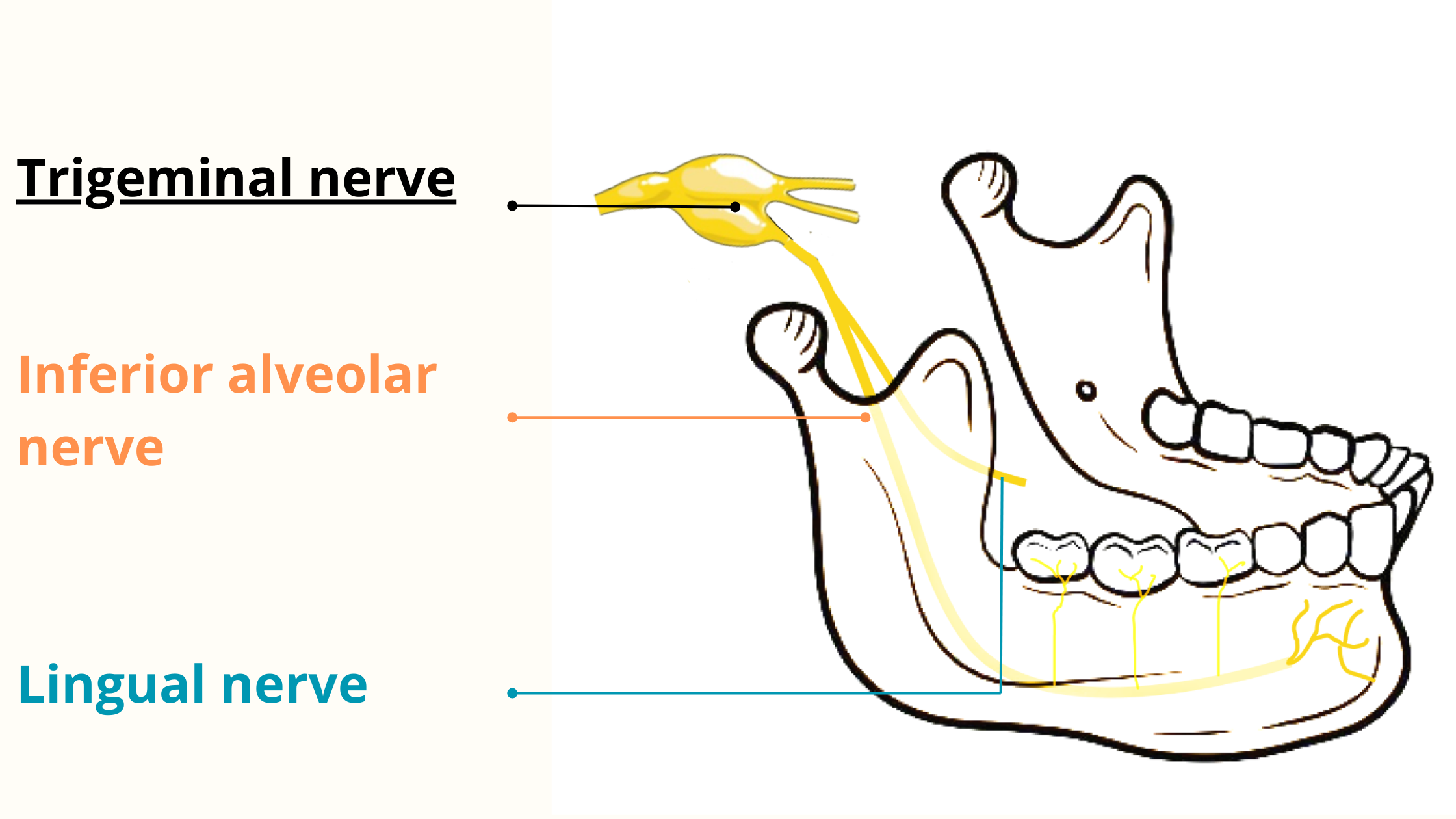

Pain signals from the teeth, jaws, and face all travel along the same nerve: the trigeminal nerve.
Whether it’s an injury, infection, or another issue affecting the mouth, teeth, or surrounding areas, the pain signals follow the same pathway to the brain. Once in the brain, they are processed and decoded — but sometimes it gets confused about where the pain is actually coming from.
This overlap and convergence of pain signals make it difficult to pinpoint the exact source of the pain. As a result, you might feel pain in one area, even though the real issue is somewhere else. This is known as referred pain.
For example, a problem with your jaw joint or facial muscles might feel like a toothache, even if your teeth are perfectly healthy. Another classic example is a heart attack — the heart is the true source of pain, but it’s often felt in the arm, shoulder, neck, or jaw.
Other Than Cavities, What May Be Causing Tooth Pain? (5 Potential Reasons)
Cavities are a common cause of toothache—but they’re not the only ones. Many other conditions can trigger pain that feels just like tooth decay, even when your teeth are cavity-free.Here are the most common culprits:
1. Gum Disease
Gum disease, also known as periodontal disease, is one of the most widespread health conditions globally, and the leading cause of tooth loss in adults.
It damages the gums and bone that support your teeth and can lead to increased tooth sensitivity, especially when eating or drinking hot, cold, or sour items.
A common cause of this sensitivity is gum recession. When the gums pull away from the teeth, they expose the tooth roots, which aren’t meant to handle the harsh environment of the mouth. These roots break down more easily and leave the underlying nerves exposed.
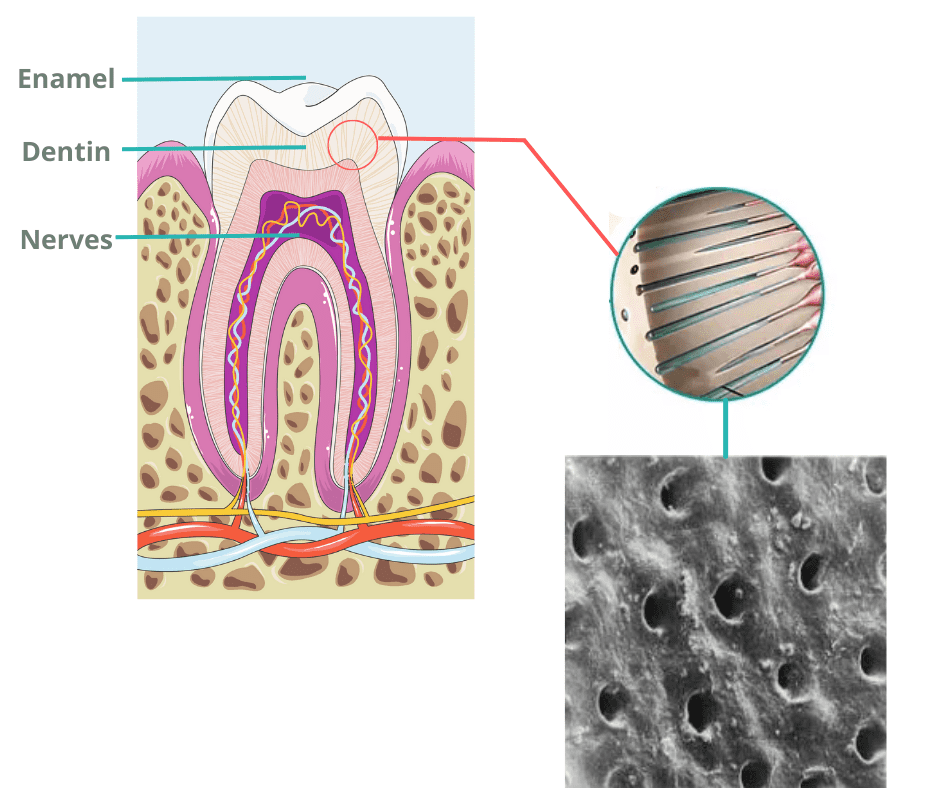
As a result, simple daily activities like sipping cold water or even breathing through your mouth can overstimulate these nerves and cause sharp, sudden pain.
Another way gum disease can lead to toothache is through infection. When the gums become swollen and inflamed—often because of trapped food or debris—the pain can spread from the gums to the teeth and even spread throughout the jaw.
2. Dental Wear
Tooth wear is another common cause of tooth pain and sensitivity. It happens when the hard outer layers of your teeth break down and become thinner, leaving the inner nerves more exposed to the mouth.
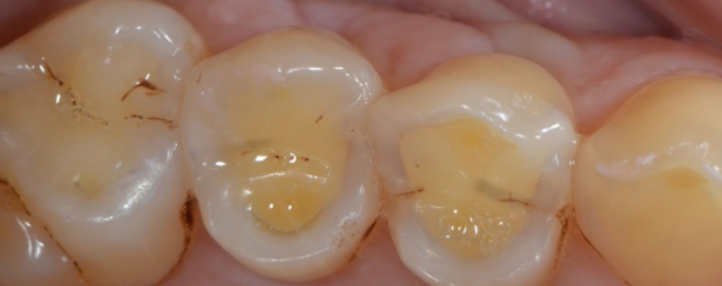
Unlike cavities, tooth wear doesn’t involve bacteria and doesn’t create visible dark holes. It’s caused by prolonged mechanical or chemical irritation, without any infection.
Similar to gum recession, worn-down teeth can become extra sensitive to hot or cold foods and drinks. In some cases, the pain can be sharp enough to make chewing difficult.
Here are some of the most common causes of dental wear:
- Teeth grinding or clenching (also called bruxism)
- Brushing too hard, especially with a hard-bristled toothbrush
- Frequent vomiting
- Chronic acid reflux (stomach acid reaching the mouth)
- The bad habit of sucking on citrus fruits or keeping them in your mouth for too long—the high acidity gradually erodes the enamel
3. Tooth Trauma
Teeth can crack or break under pressure—like when you accidentally bite down on something hard or experience an injury to the face or jaw.
Sometimes, these cracks can be tricky to spot. They can be so tiny that they’re invisible to the naked eye or don’t show up clearly on X-rays.
A common test to spot such injuries is the bite test. Try biting down firmly, then slowly release. If you feel a sharp pain right as you let go, there’s a good chance you’re dealing with a cracked or fractured tooth.
Symptoms can vary from mild discomfort while chewing to sharp, intense pain. If left untreated, a cracked tooth can allow bacteria to enter the inner layers of the tooth, leading to infection and abscess.
4. Excessive Biting Forces (Occlusal Trauma)
Your teeth—and the structures that support them, like the gums, bone, and ligaments—are built to handle a certain amount of pressure. But when that pressure goes beyond their limits, damage results.
A common situation is when a tooth sits higher than the others teeth. This causes it to take more force during chewing, stretching the ligaments and overstimulating the bone. Over time, this can lead to pain, increased wear, and even tooth mobility.
The same can happen after a filling or other dental work. If a filling or crown is too high, it puts extra pressure on that tooth every time you bite, leading to discomfort.
Everyday habits like biting on pens, chewing ice cubes, or grinding and clenching your teeth (bruxism) can also overload your teeth and supporting tissues. If you grind your teeth at night, you may wake up with increased muscle soreness, tooth pain, and headaches.
Some studies have shown that excessive biting forces may even trigger inflammation inside the tooth—similar to what happens with tooth decay.
5. Tooth Pain That Doesn’t Come from the Tooth Itself (Referred Pain)
Referred pain is when you feel pain in one part of your body, even though the actual problem is somewhere else. When it comes to the mouth, this means you could have an issue in your muscles or joints—but feel it as a toothache.
It’s more common than you might think, yet it often goes unnoticed—even by dentists!
Muscle and Joint Pain
The most frequent source of non-dental tooth pain is a problem with the muscles and joints that control your jaw, known as temporomandibular disorder (TMD).
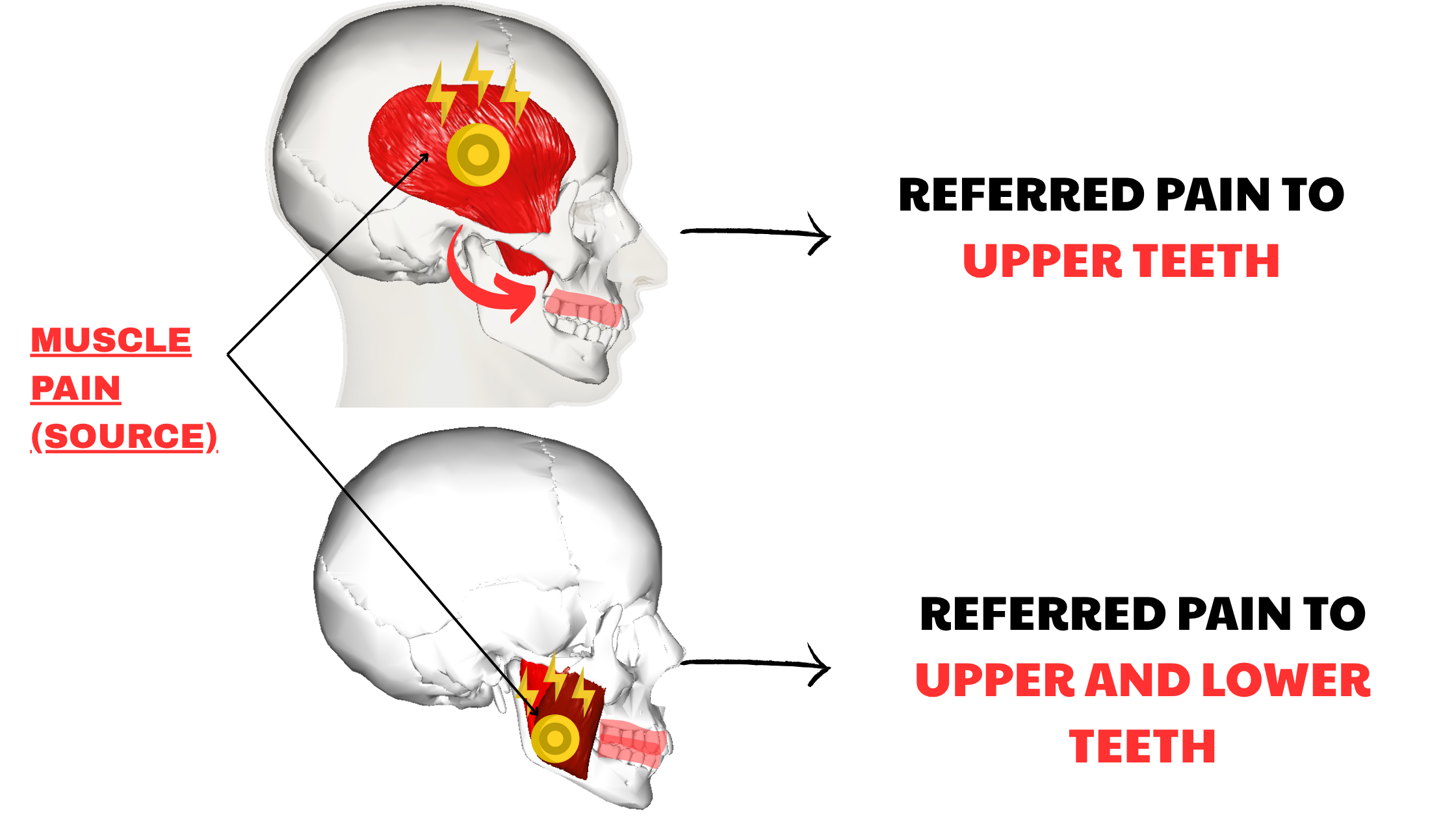
These muscles and joints help you speak, chew, and move your jaw. When they’re not working properly, they can cause deep, constant pain that gets worse with jaw movement. This pain can spread to your teeth and feel exactly like a toothache—making it easy to mistake the source.
If you're dealing with TMD, you might also notice:
- Difficulty opening your mouth fully
- A clicking or popping sound when opening your jaw
- Morning headaches
- Jaw stiffness or tightness
- Tired-feeling facial muscles
- Pain that radiates to your cheeks, temples, or ears
Sinus Pain
Your sinuses are air-filled cavities located near your cheeks, forehead, and behind your nose. When these become inflamed—a condition known as sinusitis—you may feel pressure and pain in various parts of your face.
Sinusitis can be caused by allergies, polyps, a cold, or other types of infections. Common symptoms include:
- Facial pain or pressure (especially around the cheeks)
- Headache
- Stuffy or runny nose
- Post-nasal drip
- A feeling of fullness or tightness in the face
Because the roots of your upper back teeth sit very close to the sinuses, sinus inflammation can sometimes cause pain in those teeth. This is known as sinus toothache.
It’s a type of referred pain that feels like a dental issue, even though the teeth themselves are perfectly healthy.
Cervical Issues
Problems with the cervical spine (the neck area) or surrounding muscles can also cause pain that radiates to the jaw and teeth.
Muscle tension, nerve compression, or cervical spine disorders may lead to discomfort that mimics a toothache.
That’s why, when no clear dental cause is found, it’s important to rule out cervical problems as a potential source of the pain.
Should You See Your Dentist?
If you have a toothache but don’t see any cavities, that alone is a good reason to visit your dentist. As we’ve seen, some conditions or injuries can hide well and still cause tooth pain.Your dentist will check not only your teeth but also the surrounding muscles, joints, sinuses, and even your neck—because all these areas can contribute to tooth pain.
That said, the pain might still be caused by a cavity you haven’t noticed yet. Cavities often hide in hard-to-see places, like between your teeth or on the back surfaces.
Before ruling out a cavity completely, here are a few simple checks you can try at home:
- After drying your tooth and shining a light on it, look closely for any color changes. Dark spots or stains can be a sign of decay.
- Use dental floss to clean between your teeth. If the floss tears easily or if the tooth surface feels rough or uneven instead of smooth, there might be a cavity forming between your teeth.
- The inner side of your teeth can be hard to see. Ask someone to help check for any dark stains, holes, or unusual changes in these areas.