Lump in the Cheek After Wisdom Teeth Removal: Should You Worry?

A lump or swelling in the cheek after wisdom tooth removal is completely normal, especially within the first week.
However, it's often too early to jump to conclusions at this time, as it can be hard to tell whether swelling is just part of healing or an early sign of a complication, like an infection.
Everyone responds differently to the procedure, and postoperative reactions can be quite unpredictable. So, your natural recovery won’t look exactly the same as others.
As a general rule, if a sign lasts unusually long or worsens instead of resolving, don't wait—talk to your dentist as soon as possible.
In this article, we’ll focus on one of the most common concerns after wisdom tooth removal: a lump or swelling in the cheek or around the mouth.
However, it's often too early to jump to conclusions at this time, as it can be hard to tell whether swelling is just part of healing or an early sign of a complication, like an infection.
Everyone responds differently to the procedure, and postoperative reactions can be quite unpredictable. So, your natural recovery won’t look exactly the same as others.
As a general rule, if a sign lasts unusually long or worsens instead of resolving, don't wait—talk to your dentist as soon as possible.
In this article, we’ll focus on one of the most common concerns after wisdom tooth removal: a lump or swelling in the cheek or around the mouth.
In this article:
- Chances are it's an Edema
- Hematoma: When Bleeding Goes the Wrong Way
- The Lump May Point to an Infection
- Swollen Lymph Nodes
Most Common Causes of a Lump or Swelling After Wisdom Teeth Removal
If you've noticed a lump or any form of swelling after your wisdom teeth removal, don't panic—it's completely expected during the healing process.Most of the time, these are temporary reactions and part of the body's natural response to surgery. They should resolve themselves within a week or two.
However, if the lump is getting bigger or worse over time, then it's worth talking to your dentist.
Here are the most likely causes of a lump in the cheeks after wisdom teeth extraction:
1. Chances Are, It’s Post-Surgical Edema
One of the most common reasons for lump or swelling after surgery is edema. It’s a natural reaction and happens after almost any kind of surgery.
Following wisdom tooth removal, the blood vessels in the area expand to bring in essential cells and nutrients to help with healing. This process leads to redness, warmth, tenderness, and noticeable swelling around the surgical site. The swelling can spread to other facial areas like your cheeks, lips, chin, and even under the jaw.
How bad the swelling looks can vary from person to person. Some people barely notice it, while others may feel like their entire mouth is puffed up.
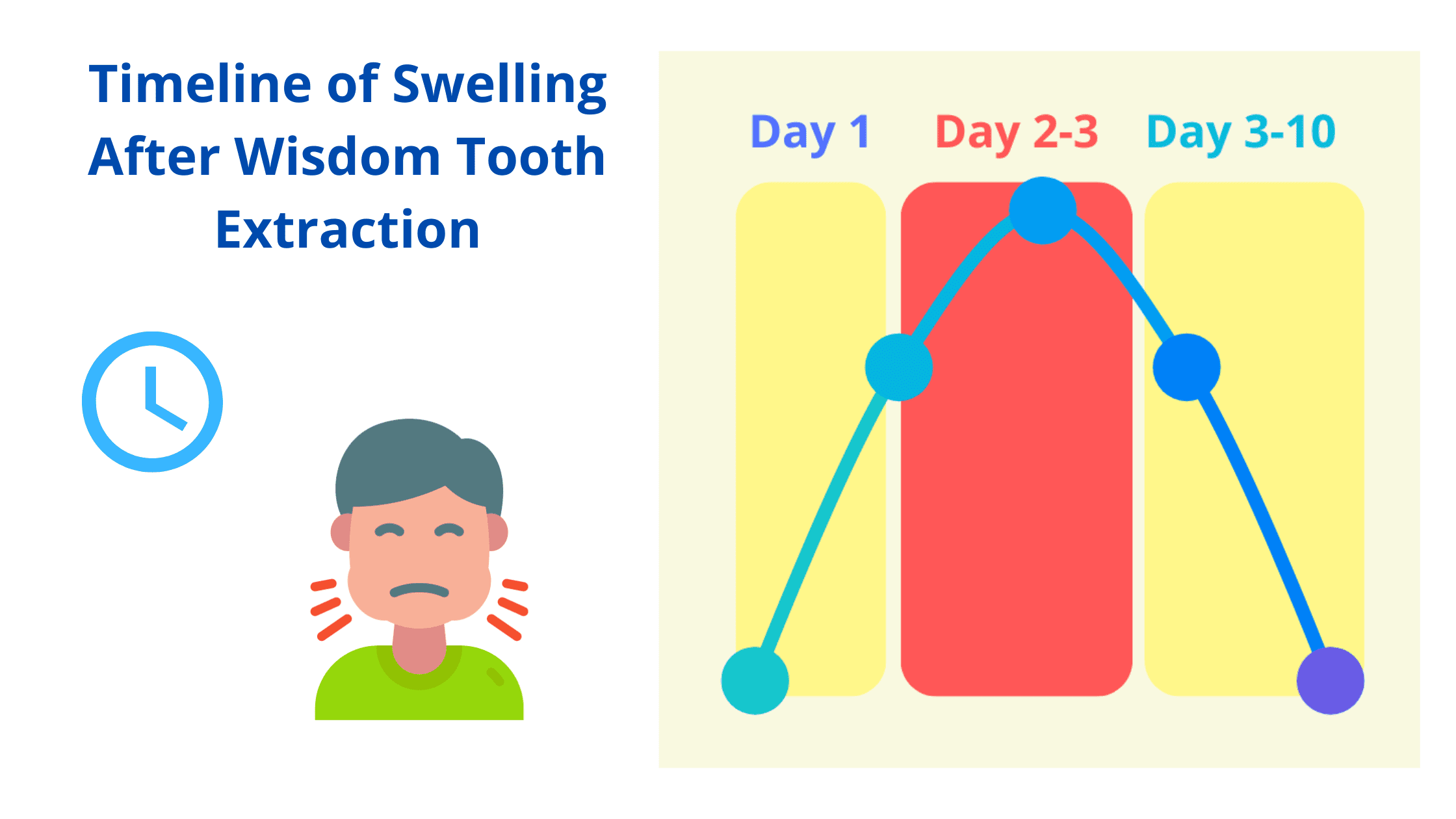
Typically, edema starts within the first 24 hours after the procedure, reaches its peak around 48-72 hours, and gradually fades within 7-10 days post-surgery.
Tips to Reduce Edema
Here are some tips to reduce edema after wisdom tooth removal:
- Ice Application in the First 24 Hours: Apply ice to the area for 20 minutes every hour during the initial 24 hours. Always wrap the ice in a cloth or towel (to avoid burning your skin). Don't go beyond the first day, as excessive cold can constrict blood vessels too much and slow down healing.
- Transition to Warm Compresses after 24 Hours: After the first 24-hour, switch to warm, moist compresses, as cold is no longer effective.
- Adjust Sleeping Posture: For the first two nights post-surgery, keep your head slightly elevated while sleeping. This will help keep the pressure in your head low.
2. Hematoma: When Bleeding Goes the Wrong Way
If you're noticing skin discoloration after your wisdom teeth removal, it's called bruising—a temporary and totally harmless pooling of blood that has leaked into the deep soft tissues.
In some cases, blood can collect in one area under the skin, forming a spongy, rubbery lump called Hematoma. It often looks bluish but can also appear black, green, or yellow as it heals.
It can look alarming by appearance, but it is temporary and should resolve on its own within 5 to 10 days.
Speeding Up Hematoma Removal
The good news is that hematomas naturally fade away as the body absorbs and eliminates the pooled blood. The same tips used for swelling (ice, warmth, and proper sleep posture) will also help bruises resolve more quickly.
3. The Lump May Signal an Infection
Complications after wisdom tooth removal are rare, but it’s always good to know the telltale signs so you understand what’s happening and what to do.
Infection is one of the most common complications. It often shows up as a lump or swelling in the cheek or around the extraction site.
Most infections begin early, within the first week, and settle within the empty socket (where the tooth used to be). Common signs include:
- A socket filled with white, brown, or gray substance
- Pus (yellowish fluid) coming from the area
- Throbbing pain
- Bad breath or a foul taste
- Fever
- Swollen lymph nodes under the jaw
- Difficulty in fully opening your mouth (though it can be a temporary side effect)
When are infections more likely to develop? If your tooth was already severely infected or abscessed before removal.
If untreated, the infection can spread—either deeper into the jawbone or, more likely, to the gums or into the soft tissues of the face (cheeks, lips, or under the tongue).
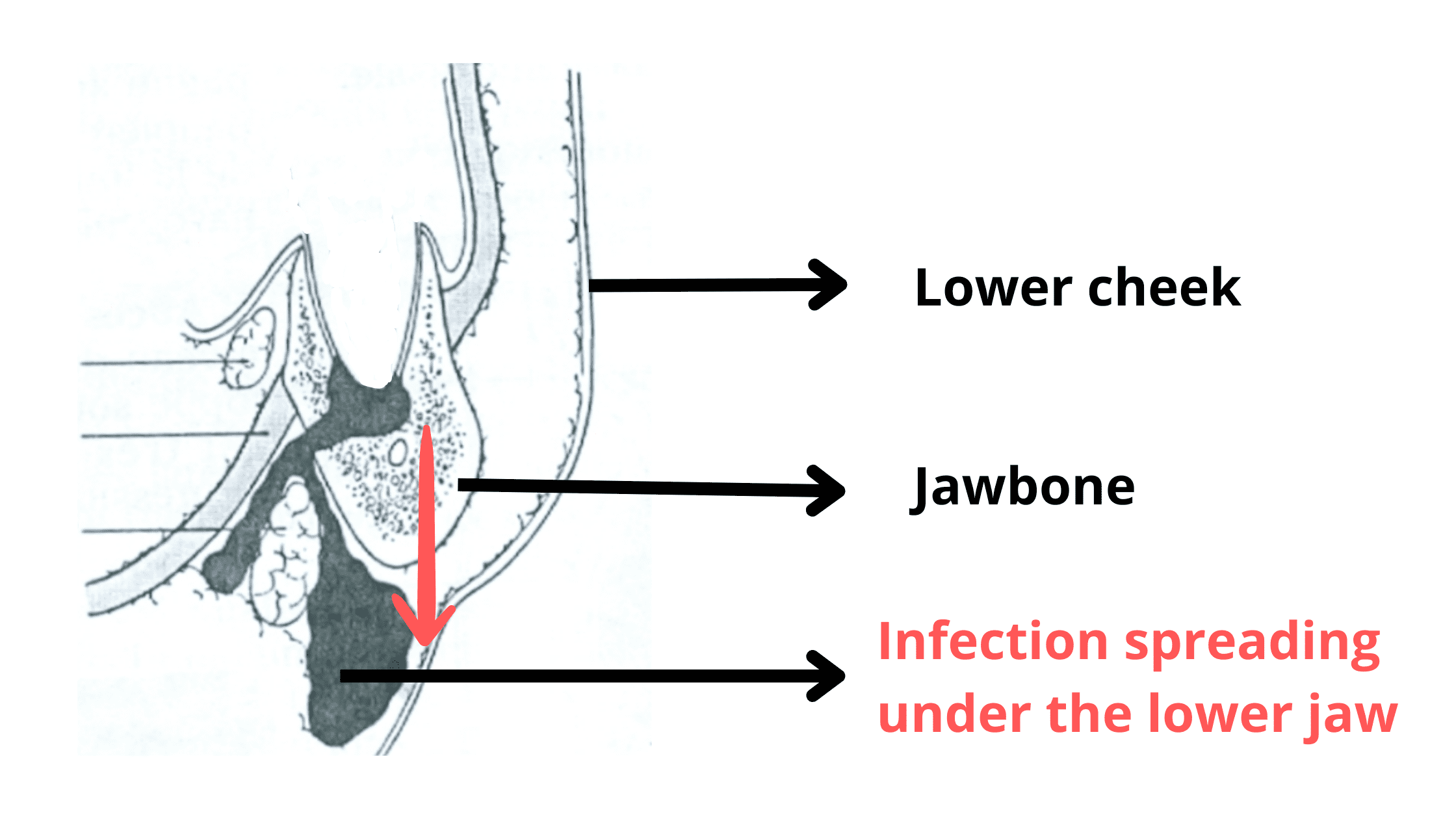
If an infection spreads to the cheek area, the swelling will first appear diffuse and widespread. After a few days, pus starts to collect in one spot, forming a noticeable lump or pimple known as an abscess.
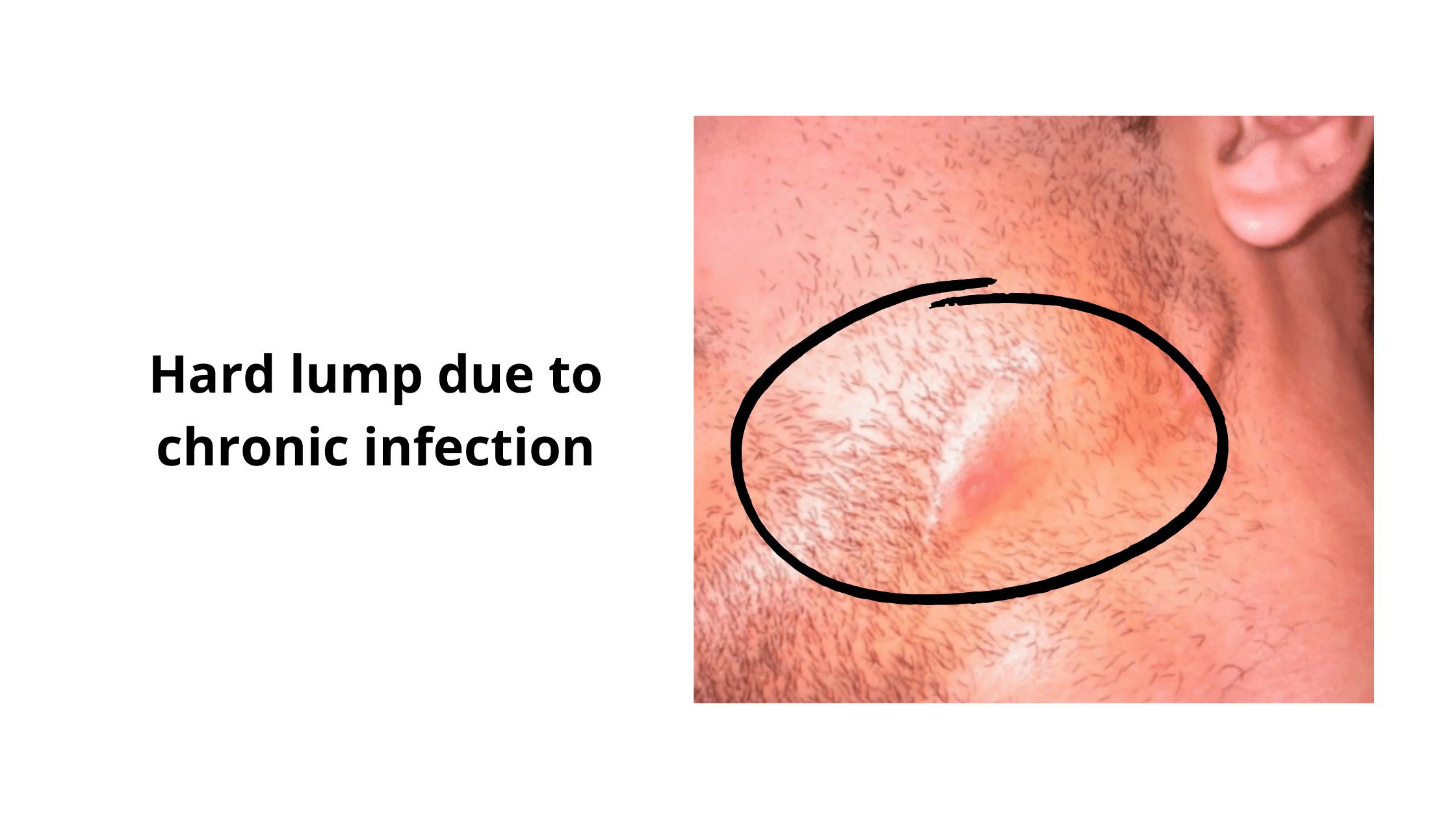
If the infection isn't treated, it can turn into a chronic problem (as shown below). The pus may harden into a firm, purplish lump. In some cases, it can drain through the skin by forming a small tunnel called a fistula.
Other factors that increase the risk of infection after wisdom tooth removal:
- Longer and more complex procedures: The more time it takes to remove the tooth and the more bone that’s removed, the higher the risk of postoperative complications.
- Lower vs. upper wisdom teeth: Lower wisdom teeth typically carry a higher risk of complications than upper ones. Why? Because the lower jaw naturally has less blood supply and is slower to heal.
- Something stuck in the wound: If a foreign object or bone fragment becomes trapped in the wound, it can lead to infection. Similarly, eating hard or crunchy foods too soon after the procedure can cause food to get stuck in the socket.
Infection vs. Normal Healing
It can be difficult to tell the difference between the early stages of an infection and the normal postoperative side effects, as both can cause swelling, redness, and mild pain.
The warning signs you should watch out for are:
- The wound is filled with a gray or black substance.
- Pus is oozing from or near the extraction site.
- A persistent bad breath and taste.
- Systemic signs like fever, fatigue, chills, and swollen lymph nodes under the jaw. These should never be ignored, as they indicate the infection is spreading.
- Symptoms getting worse rather than improving.
- Symptoms that suddenly returned.
How is Infection After Wisdom Tooth Removal Treated?
If you suspect an infection, see your dentist as soon as possible to prevent it from progressing.
Postoperative infections are usually treated with local debridement and antibiotics, often combined with anti-inflammatory medication and painkillers.
If the infection has formed a well-defined lump or abscess in your gums or cheek, your dentist may need to make a small incision to drain the pus.
Preventing Infections
It’s always better to prevent an infection than to have to cure it. Follow all prescribed medications, including antibiotics, exactly as directed. Never stop halfway, even if you feel better.
From the second day on, start rinsing with warm salt water several times a day to reduce swelling and bacterial load in your mouth.
Maintain good oral hygiene, but avoid the extraction site during the first week.
4. Swollen Lymph Nodes
Lymph nodes are small lumps, scattered throughout the body and usually too tiny to feel. They consist of immune white blood cells that help watch over the body and fight off invaders like bacteria and viruses.
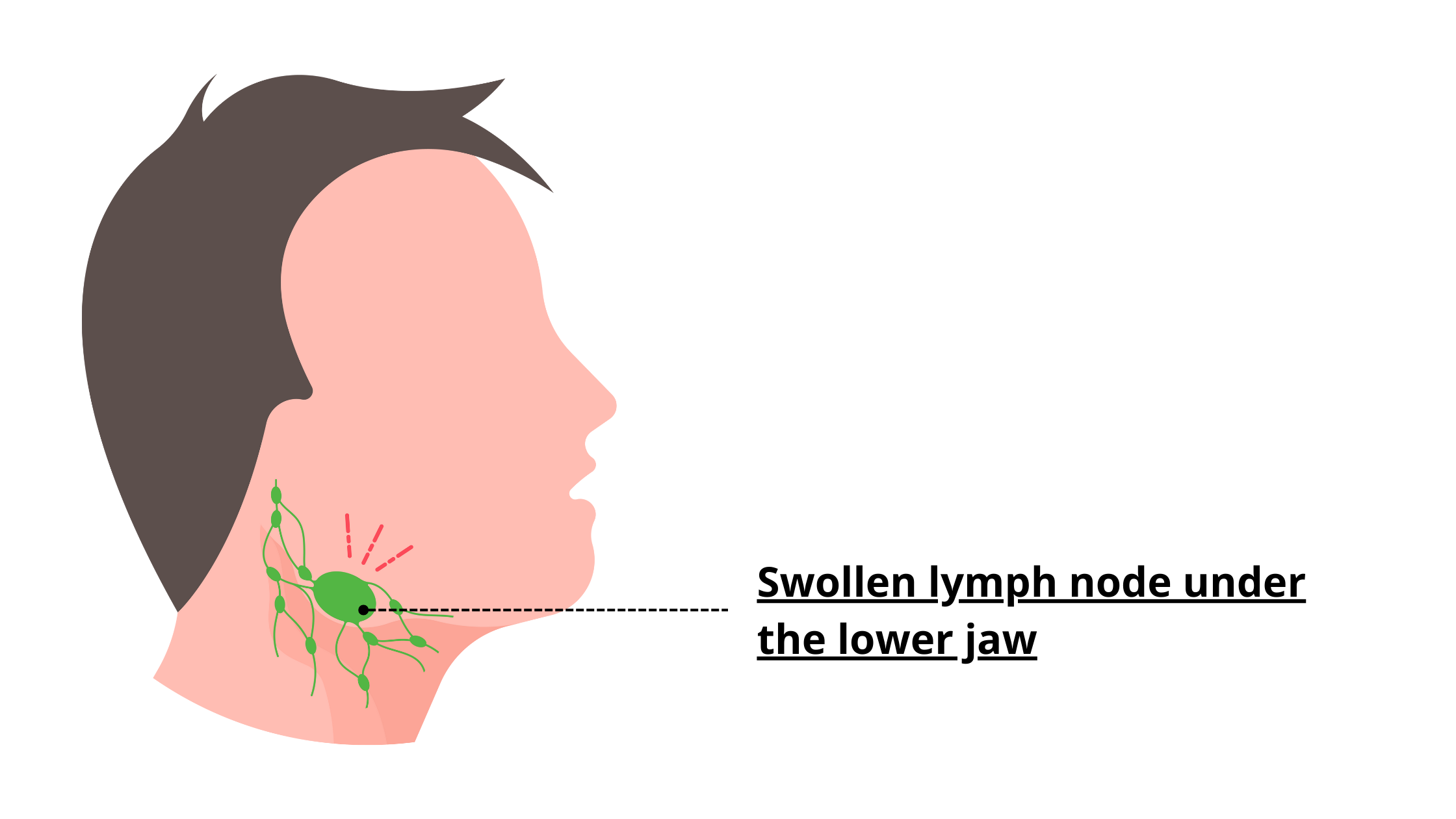
When an infection is detected, white cells multiply rapidly, causing the lymph nodes to increase in volume, becoming palpable and noticeable.
An infection after wisdom tooth extraction can cause the nearby lymph nodes—especially those under the lower jaw along the jawline—to become swollen and active. You may notice the following signs:
- The growth is bean-shaped and has clear borders.
- The size is about half an inch.
- The growth is soft and moves when lightly pressed.
- Swollen lymph nodes associated with infection are often painful.
How to Manage Swollen Lymph Nodes?
Swollen lymph nodes are just a symptom, not the problem itself. Once the infection is treated and resolved, the lymph nodes will shrink back to their normal size.
The Lump May Actually Arise From the Jawbone (rare causes)
If the wound or socket becomes infected, the infection usually spreads along the path of least resistance—often the gums and soft facial tissues. In rare cases, it can spread deeper into the jawbone.Two potential complications that arise from the jawbone include osteomyelitis and cysts:
Osteomyelitis:
Untreated infections can sometimes reach the jawbone, causing a condition called osteomyelitis. The progression may look like this:
- Initially, inflammation inside the jawbone causes hard, firm, and painful swelling near the extraction site.
- Within 2 to 3 days, pus may start to accumulate. Severe symptoms can then appear, including fever, fatigue, and a general feeling of illness. The skin and gums around the area may become red, swollen, and tender.
- Eventually, the pus may drain into the mouth, bringing temporary relief. However, this does not solve the source of the infection (which is deep within the bone). Without proper treatment, the infection can persist and damage a significant portion of the jawbone.
Jawbone cyst:
A cyst is another rare complication that affects the jawbone, often showing up as a hard lump.
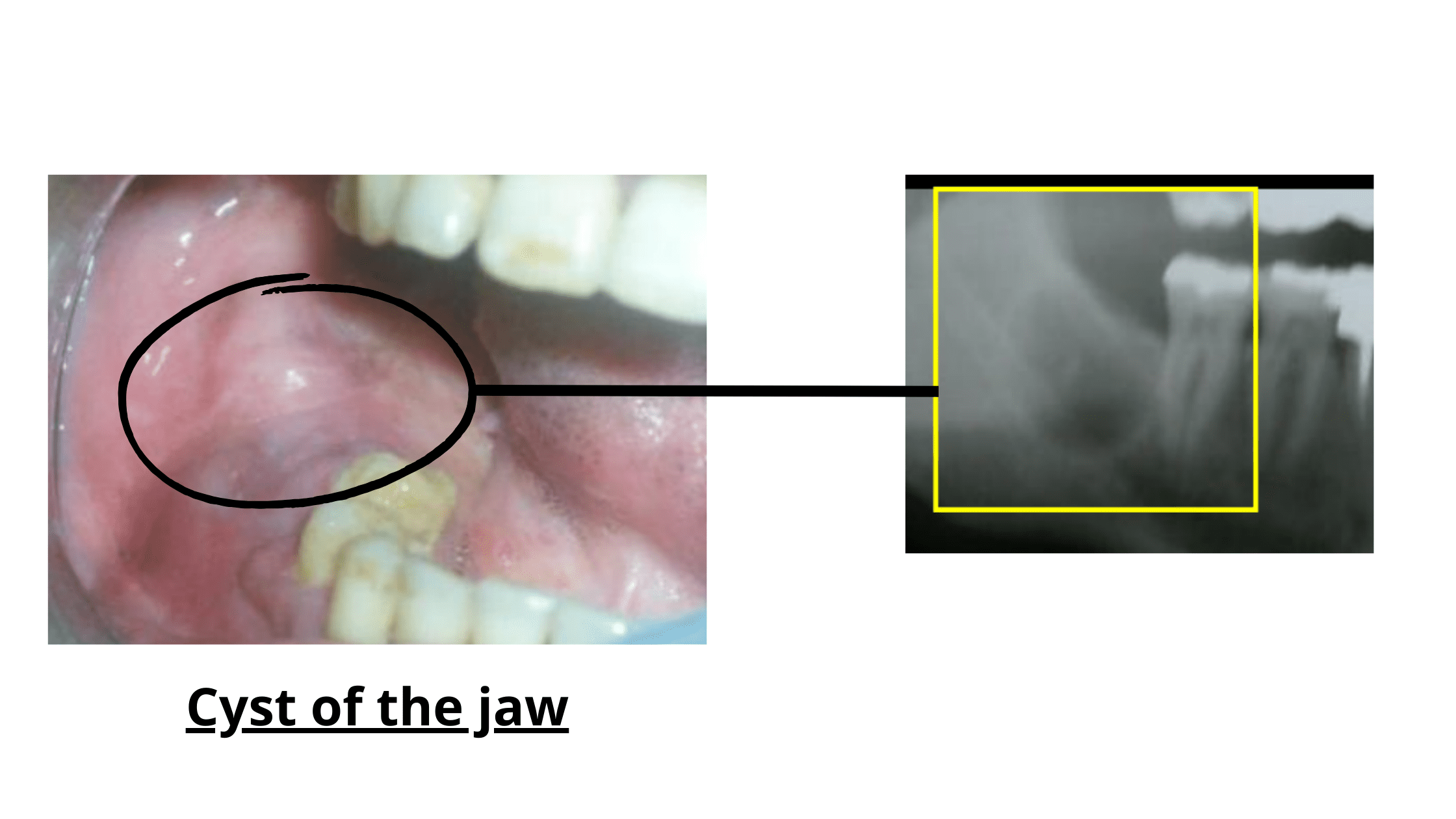
Wisdom teeth are more prone to developing cysts than other teeth. Sometimes a cyst can be missed by the dentist during the extraction. If that happens, it can remain and continue to grow.
Unlike other complications, cysts grow slowly over months or even years, often remaining painless at first. Over time, however, they can reach a significant size, potentially deforming the jawbone and causing facial issues.
A Lump After Wisdom Teeth Removal is Often Temporary
Again, the lump or swelling you're noticing in the first two weeks after surgery is likely normal and temporary. It's often the result of natural healing responses like edema, bruising, or blood pooling—all common after a surgical procedure.Rather than constantly overthinking the surgical area, focus on getting rest and carefully following your dentist’s post-op instructions.
While these side effects should naturally improve and regress over time, if they persist longer than two weeks or worsen, don't hesitate to contact your dentist or surgeon. They’re in the best position to determine what’s normal and what could be a problem for you.
When to Worry?
Swelling or lump associated with symptoms like pus leakage, fever, fatigue, swollen lymph nodes, throbbing pain, difficulty breathing and opening the mouth are warning signs of a spreading infection. Don’t ignore these — the longer you wait, the more the infection can spread, and the worse it may become.A rarer complication to watch for is subcutaneous emphysema. This occurs when air enters the wound and spreads under the skin of the face and neck, leading to noticeable swelling.
Subcutaneous emphysema usually appears suddenly, or within a few hours after the procedure, as a severe swelling. A typical sign is a crackling or popping sensation when the area is touched, caused by trapped air. It’s mostly harmless and temporary, but in rare cases, the air can travel to vital areas such as the heart or lungs.
These complications are rare and mostly preventable. Avoid coughing, smoking, or blowing forcefully during the first two days after surgery.
Doing so not only prevents air from escaping into unwanted areas but also helps keep the blood clot in place. This clot stops bleeding, promotes healing, and protects against a painful and common complication known as dry socket.